The information on this page is not meant to be a substitute for veterinary care. Always follow the instructions provided by your veterinarian.
8 Cat Diseases you Can Prevent with Vaccination and Deworming
1. Rabies (this can be spread to people)
2. Feline panleukopenia (feline distemper)
3. Feline herpesvirus infection
4. Feline calicivirus infection
5. Feline leukemia (FeLV)
6. Feline immunodeficiency virus (FIV) infection
7. Heartworm disease
8. Intestinal worms (roundworms, hookworms, whipworms, tapeworms, etc., some of which can also infect people)
12 Dog Diseases You Can Combat with Vaccination and Deworming
12 Dog Diseases You Can Combat with Vaccination and Deworming
1. Rabies (this can be spread to people)
2. Canine parvovirus infection ("parvo")
3. Canine distemper
4. Leptospirosis
5. Canine adenovirus-2
6. Canine parainfluenza
7. Canine enteric coronavirus
8. Canine influenza
9. Lyme disease
10. Bordetella ("kennel cough")
11. Heartworm disease
12. Intestinal worms (roundworms, hookworms, whipworms, tapeworms, etc., some of which can also infect people)
What You Should Know About Preventing Fleas and Ticks
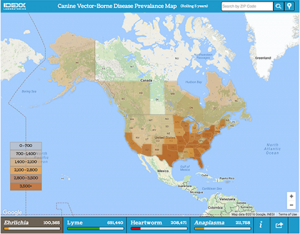
Click the map below to learn more about vector-borne disease in our area
The thought of insects crawling on your skin and living off your blood probably, well, makes your skin crawl. Yet, too often as pet owners, we allow fleas and ticks to treat our pets like bed-and-breakfasts. And it is only after these pests make themselves at home that we might realize showing them the door can be difficult, expensive and painfully slow.
Fleas and ticks aren’t just irritating and distasteful; they can lead to medical problems. Flea allergies can cause severe itching and skin damage; fleas can also carry the causative agents of cat-scratch disease, while ticks carry the organisms that can lead to debilitating illnesses like Lyme disease and Rocky Mountain spotted fever. So it’s crucial to continuously and effectively prevent infestations of these parasites for the health and safety of our pets, our families and ourselves.
Consider the life cycle of the common flea: The average female can lay 40 to 50 eggs daily. The eggs develop into maggot-like larvae and progress to a cocoon stage called pupae. These pupae wait several weeks to months for the ideal temperature and humidity to mature into adult fleas. That single adult flea you find on your pet represents about 5 percent of the total flea problem in your home; eggs, larvae, and pupae comprise the rest. Your pet — and your home — can be infested before a single flea is found. And finding them can be tough, especially on cats, because of their constant grooming. That’s why a one-time treatment for fleas isn’t usually enough. Pet owners often discover a flea problem because of a pet’s severe itching, which sometimes is due to flea allergy dermatitis — a sensitization to the flea’s saliva when it draws a blood meal. No pet is safe from fleas and their bites, but not all pets are hypersensitive to them. This means severe infestations can occur without your dog or cat showing any obvious discomfort. Therefore, it’s best to use preventive tactics to help keep fleas from infesting your pet and home in the first place. To do this, speak with your veterinarian about safe flea-control products that you can administer to your pet year-round. Some products are administered once a month, but other products provide longer-lasting protection. Ask your vet about the best choice for your pets. Consistent use of safe prevention products is the primary method of managing fleas. Newly hatched young adult fleas usually feed right away. If your pet has been treated with an appropriate flea product when these adult fleas emerge, you can help break the cycle of infestation. (Remember to treat all of the pets in the house, regardless of whether or not they’re itching.) Treating your pet’s environment is also an important part of controlling and preventing flea infestations. Fleas lay their eggs on your pet, but the eggs usually fall off. Once in the environment, they molt into larvae and develop into the pupae stage. Larvae don’t survive well in sunlight, preferring instead to hide in dark, protected areas like deep carpet or pet bedding. Therefore, focus on treating the places your pet likes to rest, especially those that are out of sunlight, like a resting place in the shady area of the yard, your pet’s blanket or pillow — or even your bed (ick). Frequent cleaning or vacuuming can help reduce the pupal and larval stages of fleas in the carpet, and many flea control products used on pets also kill eggs and larvae. But don’t forget that fleas can gain access to your house or yard in many ways, including wildlife, neighborhood cats and you, just to name a few. Also remember that if your dogs or cats are allowed access to other areas — such as parks, nature areas, crawl spaces or even the neighbor’s yard — they’ll have ample opportunity to encounter fleas. Therefore, even if you’re treating your pet, areas of your home and yard may also need regular attention. Like fleas, ticks can now be found throughout most of the country. Though the severity of tick infestations varies by region, ticks are now spreading into areas that previously had very limited tick problems. Unlike fleas, ticks may not cause dramatic irritation when they attach to your pet’s skin. This lets the tick slowly fill with blood without interference. Before feeding, ticks are often small and easily overlooked; once a tick has eaten and is engorged with blood, it grows in size and often looks bloated. These bloated ticks are usually easier to spot (depending on species—some of them can still be very small), but can be difficult to remove —especially if you aren't used to doing it. If you see a bloated tick, your best bet is to visit your veterinarian so she can remove it and check for any additional ticks. There are several species of ticks that pose a risk to pets and people. Ticks can be hosts to several types of disease-producing organisms that can be transmitted to pets or people while the tick is feeding. These organisms can cause illnesses like Lyme disease and Rocky Mountain spotted fever. Again, the lesson here is that it’s best to protect your pets — and yourself — from ticks rather than react to them after the fact. Most ticks lurk in tall grass or low-hanging bushes and crawl onto pets or people as they walk by. The tick can then travel on the host — that’s you or your pet — to find a suitable place to attach and feed. Considering how stealthy these travelers are, the most reliable plan is to keep your pet on an effective tick preventive all year. Conveniently, many products combine protection from ticks with flea protection. Your veterinarian can recommend a product that is safe and appropriate for your pet. You can also help prevent ticks by keeping the grass and bushes in your pet’s outdoor area mowed and trimmed. If you’re hiking, camping or playing in untended and possibly tick-infested outdoor areas, wear long pants, long-sleeved shirts and headgear to help prevent tick exposure. Afterward, be sure to check both your pets and your family for ticks. Some circumstances may seem like they’d be guaranteed flea and tick free, but this is not so. There is no such thing as a completely risk-free situation. Pets need prevention in every situation. Think your indoor pet is safe? Think again. You’ve seen bugs inside your house — fleas and ticks can sneak indoors, too. Even pets who don’t venture outside — such as an indoor cat or a dog who only goes in the yard for potty breaks — are at risk of flea and tick infestation. Granted, their infestation chances are lower than those of outdoor pets, but you can help protect them by using safe and effective flea and tick control products year-round. And don't assume that there's a flea- and tick-free season. Fall and winter may seem like distant memories at this time of year, but they’re not to be forgotten when it comes to parasite prevention. Fleas and ticks have a way of popping up in the colder months. In fact, flea numbers can surge in the fall in temperate climates. What’s more, fleas enjoy a wonderful, climate-controlled environment inside your house year-round. They can gain inside access by hitching a ride on outside sources, such as you and your pets, or adult fleas can develop from eggs or larvae that were already hiding in your house. Don’t forget that ticks are extremely tough, too, and can often survive outside even during the winter months. The only way to ensure your dog or cat is safe from fleas and ticks is to keep him on a parasite preventive all year. Today’s highly effective parasite preventives each work a little differently to keep fleas off your pets; your veterinarian can recommend a product that best suits your pet’s health needs and your lifestyle. Here’s a look at the differences between oral products (which your pet eats) and topical products (which you apply to your pet’s skin). There are also some effective collars that you may want to ask your vet about. Oral Flea Control Topical Flea Control Remember this mantra: When it comes to fleas and ticks, it’s best — and safest — to prevent an infestation than it is to deal with the consequences. Your veterinarian, as an expert in parasite control and prevention, can recommend the best products to help prevent infestation. (Keep in mind that not all insecticides are safe for both cats and dogs of all sizes, so carefully follow your veterinarian’s recommendations.) With a little effort and a year-round prevention plan, you can keep your pets virtually parasite free — and help ensure that your home sports a “no vacancy” sign when it comes to fleas and ticks.Fleas: The Prolific, Perplexing Parasite
Ticks: Expanding Their Disease-Carrying Reach
The Risk-Free Myth
Keeping Fleas off Pets: Your Options for Preventives
Stop Fleas and Ticks Before They Start
Pet First Aid Tips
What would you do if
...your dog ate the bag of semi-sweet chocolate chips that was left out on the kitchen counter?
...your cat had a seizure right in front of you?
...your dog fell down the stairs and started limping?
...your cat was overheating on a hot summer day?
View our Pet First Aid brochure To avoid the feelings of panic that may accompany these situations, we recommend the following steps to better prepare you for a pet medical emergency. The following links summarize the basics you need for giving first aid care to your pet. Always remember that any first aid administered to your pet should be followed by immediate veterinary care. First aid care is not a substitute for veterinary care, but it may save your pet's life until it receives veterinary treatment. First aid supplies How to handle an injured pet Basic pet first aid procedures First aid when traveling with your pet Pets and disasters
Our handy checklist tells you all the supplies you should have on hand for pet first aid. Print out a copy to use for shopping, and keep a copy on your refrigerator or next to the first aid kit for your family, for quick reference in emergencies.
Knowing how to comfort an injured pet can help minimize your pet's anxiety and also protect you and your family from injury.
Read our simple instructions for providing emergency first aid if your pet is suffering from poisoning, seizures, broken bones, bleeding, burns, shock, heatstroke, choking or other urgent medical problems. Print out a copy to keep with your pet emergency kit.
A few simple steps can better prepare you to help your pet in first aid situations while you are traveling. Remember: pet medical emergencies don't just happen at home.
Whether confronted by natural disasters such as hurricanes, or unexpected catastrophes such as a house fire, you need to be prepared to take care of your animals. A pre-determined disaster plan will help you remain calm and think clearly.Additional pet first aid links
!!Fleas!! Myth vs Fact!
!!Fleas!! Myth vs Fact!
My house has no carpet, so I do not have to worry about fleas in my home.
Fact: Flea eggs will drop off the pet and accumulate in the cracks of hardwood floors and along the baseboards. The larvae will then move deep into these crevices to avoid exposure to light. Fleas can survive and multiply in most environments.
I do not see fleas on my pet, so there must not be any.
Fact: Visible adult fleas are only a small portion of the infestation. Fleas exist in the environment as ≈57% eggs, 34% larvae, 8% pupae, and 1% adults. Fleas are difficult to see on many types of hair coats. They can be harder to see on cats, who are very good at removing the fleas when they groom.
My pet never leaves my yard, and my lawn is short and well maintained.
Fact: Fleas will survive in any shady, moist environment where pets rest.
I do not need to use preventives during the winter months.
Fact: Fleas can survive for 10 days at 37.4oF. In cold climates, adult fleas survive on the warm bodies of dogs, cats, and other mammals, and indoors within pupal casings as pre-emerged adults.
I give my dog garlic as a natural flea preventive.
Fact: Garlic ingestion is an ineffective flea remedy that can have negative health effects. Garlic toxicity can result in oxidative damage to erythrocytes, which may lead to Heinz body formation, hemolytic anemia, methemoglobinemia, and impaired oxygen transportation.
Why you Should Not Feed Grain Free Diets
FDA Investigation into Potential Link between Certain Diets and Canine Dilated Cardiomyopathy
Check out the links below to learn more:
https://www.aaha.org/publications/newstat/articles/2021-08/new-clues-to-diet-associated-dcm-in-dogs/
Bathing Your Dog
Every pet owner has an olfactory (smell) memory that triggers their gag reflex, “I’ve never smelled anything like it! (S)He must have rolled in something dead!Odors that defy classification have an obvious solution; bathe the dog. Soap choice is where the confusion starts. In some situations it seems nothing but the harshest solvents will be adequate to clean your pet. It may also seem reasonable to use dish soap or a product designed for human hygiene, such as shampoo. “Harsh chemicals aren’t necessary,” assured Terese DeManuelle, a veterinary dermatologist from Portland, Oregon. “A mild hypoallergenic soap that’s formulated for veterinary use is all you need.” “Formulated for veterinary use” means a product that’s designed to work with a dog’s body. While dish soap or your favorite shampoo might strip away the dirt, and more importantly the odor, from your pet’s coat, it will also strip natural oils from their fur and may irritate their skin.
All grooming products (human and animal) are designed to maximize cleaning and minimize irritation. Human products work best on human skin and veterinary products are designed to work best on dog skin. The chemistry of a dog’s skin and fur are different than the chemistry of a human’s skin and hair. In addition to the odor- provoked “emergency bath” Dr. DeManuelle notes it’s safe to bathe your dog with veterinary shampoo once a week. However, if the veterinary shampoo you’re using contains any medication or insecticide, follow the instructions provided by your veterinarian. Prescription shampoos treat specific problems and may necessitate bathing more or less frequently than once a week. A final insight pertaining to bathing your pet is to comb their coat prior to bathing. Wet fur mats more than dry fur so a wet tangled coat is harder to brush out and will take longer to dry. This small detail can save you time and prevent an uncomfortable brushing for your pet. After a bath your dog will smell good, look good, and probably feel good. Make sure your dog is dry before you allow it back outside or it will feel good enough to dry itself. It will streak from the tub straight outside to find a new exotic aroma to frolic in and bring home to share. This Pet Health Topic was written by Sarah Hoggan, Washington State University, Class of 2001.
An Overview of Cancer
Cancer is caused by uncontrolled and purposeless growth of cells in the body. Other terms for cancer are malignancy, tumor and neoplasia. Cancer can arise from any tissue in the body so there are many types of cancer.
Some forms of cancer have the ability to spread to other sites in the body which are often far from the original site. This happens when cancer cells enter the blood or lymph vessels and are then carried to other organs. Cancers with this type of behavior are considered malignant.
Often, it is the spread of a cancer that causes the greatest problems. When a cancer has spread in this fashion, it is said to have metastasized. Some cancers lack the ability to metastasize, but may cause significant damage due to growth and invasion into local tissues. Tumors that do not metastasize and are not invasive are considered benign. Tumor is a general term for cancer whether it is benign (“good cancer”) or malignant (“bad cancer”). Oncology is the branch of medicine dedicated to the study of cancer, and the people treating your pet at WSU are Oncologists and Oncology nurses. The first task for the veterinarian is to determine the extent of the tumor which is a process called tumor staging. Staging information is vital for several reasons including: 1. determination of your pet’s prognosis (i.e., the expected outcome for your pet from the illness) and, To gather information that can help to determine the extent of the cancer, your veterinarian will need to evaluate your pet by several methods. These usually include blood tests (e.g., blood count, chemistry profile), urinalysis, radiographs (x-rays), tissue aspirate (a sample taken with a fine needle) and biopsy. Tests which your veterinarian may have performed might be repeated at WSU due to the changing nature of your pet’s illness. In addition, as indicated for specific patients, other testing procedures may include: ultrasound, specialized radiologic studies (e.g., CT scan, dye contrast studies), bone marrow aspirate, lymph node aspirate, endoscopy (direct examination of the stomach, colon or bronchi with a specialized scope), and immunologic studies. It is important to note that medicine is not an exact science and despite these staging procedures, it is still possible to fail to recognize small sites of tumor or the presence of tumor in organs that are difficult to study. Once the tumor staging has been completed, your veterinarian will better be able to discuss treatment options for your pet. The goal of such therapy will also be discussed. Tumors that have metastasized extensively are usually not curable. Therefore, the objective of therapy for these animals is palliation (i.e., afford relief of signs without providing cure, and possibly, prolong life). Localized tumors that are not deeply invasive have the best chance to be cured. There are several types of therapy used to treat cancer in dogs and cats at WSU. These include surgery, chemotherapy, radiation therapy, and immunotherapy. For some tumors, treatment will consist of a single type of therapy, while combination therapy may be recommended for other types of cancer or for animals with a more advanced stage of disease. On occasion, due to the rarity of a particular tumor, a precise treatment recommendation may not be known. In an effort to test newer (and hopefully more effective) forms of therapy, you may be asked to enroll your pet in an investigative clinical trial. The purpose of such a trial is to learn more about the specific type of treatment (that may be of value to humans and other pets with cancer) as well as hopefully providing a benefit to your pet. Only pet owners of animals with tumors for which there is no effective treatment, or tumors that have not responded to conventional treatment will be offered investigative therapy for their pets. Treating animals with cancer is not appropriate for every pet owner. It takes a strong commitment on the part of the owner. Therapy requires frequent trips to the veterinary hospital and can be expensive. For some forms of cancer treatment, once begun treatment is never stopped during the animal’s life although the frequency of these treatments can be decreased. Your veterinarian cannot do it alone since treating pets with cancer is truly a team effort and the pet owner is on the team. It is important for you to present your pet for treatment precisely when requested to do so by your veterinarian since the timing of cancer therapy is critical for obtaining an optimal outcome. In addition, medicines to be given to your pet at home should be administered by you exactly as instructed by your oncologist. Any abnormalities or problems you encounter should be reported to your regular veterinarian or oncologist promptly. Always feel free to ask questions and communicate with us. Keep in mind your veterinarian is as concerned about the quality of your pet’s life as you are. The goal of the therapy is to keep your pet happy and minimize discomfort. Although some animals may experience transient discomfort from therapy, treatment of most pets with cancer can be accomplished without major distress or detraction from your pet’s enjoyment of life. Just because an animal has been diagnosed with cancer does not mean its life is immediately over. Your commitment to your pet and your veterinarians dedication to providing state-of-the-art care will work together to keep your pet as happy as possible.
Tumor Evaluation (Work-up): Tumor Staging
2. formulation of a plan for treatment.Cancer Therapy
Should You Treat Your Pet?
Chronic Kidney Disease and Failure
Chronic kidney disease is defined as kidney disease that has been present for months to years. Chronic renal disease (CRD), chronic renal failure (CRF), and chronic renal insufficiency refer to the same condition.
CKD is not a single disease. There are many different causes of CKD but by the time the animal shows signs of kidney disease the cause may no longer be apparent. Some potential causes of CRF include:
Often the cause of CKD is unknown. The microscopic unit of the kidney is called the nephron. Each kidney contains thousands of nephrons. When the pet is young and healthy not all nephrons are working all of the time; some nephrons are held in reserve. As the animal ages or if the kidneys are damaged, some nephrons die and other resting nephrons take over the work of those that die. Eventually all the remaining nephrons are working. When there are no extra nephrons remaining and kidney damage continues the pet will start showing signs of CKD. Because of this stepwise loss of nephrons the kidneys are able to "hide" the fact that they are damaged until the damage is severe. When 2/3 of the nephrons have been lost the pet is no longer able to conserve water and the pet passes larger amounts of dilute urine. By the time a pet has an elevation in the waste product creatinine in its blood, 75% of the nephrons in both kidneys have been lost. When blood flows through the kidneys, the kidneys act as a complex filter that removes from blood wastes that are generated from break down of food, old cells, toxins or poisons and many drugs that are given for treatment of other diseases. The wastes are removed with water as urine. Waste products than can be measured in the blood include creatinine and urea nitrogen but there are many other waste products that are not measured by blood tests. The kidneys also acts as a filter to keep "good" substances in the blood. The kidneys regulate the amount of water in the blood by excreting extra water and retaining water to prevent dehydration by varying the amount of urine that is produced. The kidneys help regulate blood pressure by saving or eliminating sodium based on how much sodium the pet is eating. The kidneys help regulate calcium and vitamin D which keep bones strong. The kidneys produce a substance that helps with the creation of new red blood cells. Because the kidneys have so many functions, when the kidneys are not working normally, there are many signs that the pet may show. By the time the pet shows signs of CKD, the damage is severe. There is no cure for CKD. The remaining nephrons are working so hard that with time they will fail as well. CKD is usually fatal in months to years but various treatments can keep the pet comfortable and with a good quality of life for months to years. Because the kidneys perform so many functions, the signs pets with CKD show can vary quite a bit. The signs may be severe or may be subtle and slowly progressive. Despite the chronic nature of the disease, sometimes signs appear suddenly. Some of the more common signs of CKD include: Signs you may see if you examine your pet include: dehydration, weight loss, pale gums and ulcers in the mouth. The signs seen in pets with CKD and the findings on examination are not specific for CKD and may be seen with many other diseases so blood and urine tests are needed to make a diagnosis of CKD. Abnormalities that are often seen on diagnostic blood and urine tests include: Sometimes bruising occurs where the blood sample was drawn as pets with CKD may have platelets that are less sticky than normal (normal platelets prevent bruising). A diagnosis of CKD can usually be made based on the signs, physical examination and blood and urine tests but other tests may be performed to look for an underlying cause for the CKD and/or to "stage" the CKD. The severity of chronic kidney disease (CKD) can be estimated based on blood waste product elevation and abnormalities in the urine such as the presence of protein. The International Renal Interest Society (IRIS) has developed a method to estimate the stages of CKD. Stages are numbered 1 through 4 where one is the least severe and four is the most severe. The higher the stage number also generally corresponds to the greater number of symptoms seen in the pet. Some treatments are recommended to be started when the pet has a certain stage of CKD. See the IRIS site for full details on staging. The severity of the pet's signs will determine what treatments are needed. Not all treatments presented below may be needed or appropriate for each pet with a diagnosis of CKD. Treatments may also be started incrementally (a few treatments are started and then based on patient response, additional treatments may be added later). The information below is not meant to be a substitute for veterinary care. Pets with severe signs may be hospitalized for fluid and intravenous drug treatment to reduce the amount of waste products in their body. Many pets with CKD will feel better in response to treatment with IV fluids but if the kidney disease is extremely severe the pet may not respond to treatment. Those pets who are still eating and not showing severe signs are treated with a variety of treatments, often introducing treatments incrementally as new signs develop. The treatment approach is often called "conservative" compared to more aggressive treatments such as hospitalization for fluid therapy, dialysis or kidney transplantation. Remember that CKD is not a disease that can be cured. Treatments are designed to reduce the work the kidneys need to perform, to replace substances that may be too low (such as potassium) and to reduce wastes that accumulate such as urea (generated by the body from proteins) and phosphorus. The initial response to conservative therapy may be relatively slow, taking weeks to months to see a response. Diet Protein restricted diets are less palatable than higher protein diets. Pets with CKD that are still eating are more likely to accept a change in diet to a protein restricted diet than are pets who are very ill and refusing most foods. Protein restricted diets are more expensive than higher protein diets. There are many pet food companies that sell kidney diets. Dr. Tony Buffington at the Ohio State University is a good source of information on available diets. http://vet.osu.edu/1442.htm select a species, a diet form and select Reduced Phosphorous/Protein for a list of diets for pets with kidney disease. Homemade diets can be fed but it is best to work with your veterinarian to formulate a diet that is balanced. It is generally agreed that feeding renal failure diets to dogs and cats with kidney disease improves their quality of live and may minimize the progression of the disease resulting in a longer life span. Studies that evaluate the effect of dietary changes on quality and quantity of life typically use commercial diets that differ in their composition of protein, phosphorus, sodium and lipids compared to maintenance diets so that positive effects are not attributable to a single component of the diet but rather to a "diet effect". A randomized, double masked, clinical study in 38 dogs with spontaneous stage 3 or 4 kidney disease, half of which were fed a kidney failure diet and the other half a maintenance diet, published in JAVMA in 2002, demonstrated improved quality and increased quantity of life in the group fed the renal failure diet. The results of a study of cats with naturally occurring stable chronic renal failure fed a diet restricted in phosphorus and protein compared to cats with CKD fed a maintenance diet reported a median survival of 633 days for 29 cats fed the renal diet compared to 264 days for 21 cats fed a regular diet. The groups were not randomly determined but based on cat & owners willingness to change to the renal diet. In a study published in JAVMA in 2006, 45 client-owned cats with spontaneous stage 2 or 3 CKD were randomly assigned to an adult maintenance diet (23 cats) or a renal diet (22 cats) and evaluated for up to 24 months. Findings included: Water Water soluble vitamins like B and C are lost in greater amounts when the pet is urinating greater amounts. Kidney diets contain increased amounts of water soluble vitamins so additional vitamins do not need to be given unless a homemade diet is being fed. Potassium Phosphorus, calcium and PTH Kidney diets typically contain reduced phosphorus and an appropriate amount of calcium but if phosphorus remains elevated when the pet is eating a kidney diet then phosphorus can be tied up in the intestinal tract so it can be eliminated in the stool. Intestinal phosphate binding agents include aluminum carbonate, aluminum hydroxide, aluminum oxide, calcium citrate, calcium acetate and calcium carbonate and sevelamer hydrochloride. Phosphate binding agents which contain calcium should not be used until blood phosphorus is normal to prevent calcium and phosphorus from combining and precipitating in tissues including the kidneys. It is not usually necessary to give additional calcium but if a pet has low blood calcium, the phosphorus should be normalized before giving calcium. Even when blood phosphorus is normalized, PTH levels are still higher than normal. The administration of low doses of vitamin D (1, 25 dihydroxycholecalciferol [calcitriol]) will suppress PTH and possibly slow the rate of progression of kidney deterioration. It is not 100% agreed that giving your pet calcitriol will slow the deterioration of the kidneys. Here are some web sites on using calcitriol http://members.bellatlantic.net/~vze2r6qt/calcitriol/ Acidosis Sodium High blood pressure (hypertension) Anemia Anemia can be treated by blood transfusion or by the administration of human erythropoietin. Erythropoietin is very effective in increasing PCV but because human erythropoietin is not exactly the same as dog and cat erythropoietin, over time, the pet may form antibodies that cause the medication to become ineffective. Canine and feline erythropoietin are currently being studied. Fats/lipids Subcutaneous Fluids Lack of Appetite Vomiting Drugs used to treat other diseases Antibiotics You are in the best position to judge what is stressful to your pet. When a pet is stressed they may drink and eat less than normal. Reduced water intake is detrimental to diseased kidneys. When possible, keep your pet calm. That might mean for example: having an in-home pet sitter if your pet is stressed by boarding, removing the pet from the household during a party or limiting contact with other animals if these situations appear to be a source of stress for your pet. Extremes in heat or cold are stresses. Certain drugs such as prednisone/cortisone make the kidneys work harder.
Structure of the kidneys
What do the kidneys do?
CKD is progressive
Signs of CKD
Less common signs include
Diagnostic Tests
Other tests that may be performed include
What might this test show? The kidneys in pets with CRD are usually small reflecting the death of a large number of nephrons. If the kidneys are large then certain causes for the CKD should be considered such as lymphoma (cancer) of the kidneys, or an uncommon disease called amyloidosis. Some pets with signs of kidney disease who have large or normal sized kidneys may have acute kidney failure rather than CKD. The treatment and prognosis for pets with acute kidney disease differs from the treatment and prognosis of pets with CKD.
What might this test show? A biopsy is not required to make a diagnosis of CKD but the results of a biopsy may show a cause for the CKD. A biopsy is more likely to show specific information when the kidneys are big rather than small. A biopsy can be valuable in pets who develop CKD at a young age or who are of a breed known to develop congenital kidney disease. There may be specific microscopic changes in a kidney biopsy from an animal with congenital kidney disease that may suggest that related animals are also at risk for developing CKD. Knowledge that the cause of CKD is caused by congenital kidney disease does not change the treatment of the affected animal but does provide information for related animals, for example if you should remove them from a breeding program. When a biopsy is planned, usually the biopsy is collected using ultrasound or laparoscopy to see the kidney during the biopsy so that no other organs are damaged during the biopsy.
What might this test show? Bacterial infection is not a common cause of CRD but pets with CKD may develop a bacterial infection as several aspects of the pet's immune system may be less functional when the kidneys are failing. If white blood cells are observed on microscopic examination of the pet's urine, a bacterial culture of the urine should be obtained.
What might this test show? If a pet is going to under go kidney biopsy, tests may be performed in advance to evaluate the ability to stop the bleeding from the biopsy site.Treatment of CRF
Feeding of a kidney diet is usually recommended. Kidney diets contain less protein compared to other diets and the protein is high in quality. It is protein in the diet that is converted to waste products that the kidneys must remove in the urine. The higher the quality of the protein in the diet, the less wastes created for the kidneys to eliminate. Low quality protein requires the kidneys remove more wastes. which makes them work harder. Egg and meat contain higher quality protein; cereal grain protein is of lower quality which leads to more wastes for the kidneys to eliminate. Protein is used by the body to repair cells and tissues that are continually regenerating, so a pet needs some protein in their diet. By feeding a low quantity, but high quality protein diet that contains an appropriate amount of fats and carbohydrates, the pet's body can use the protein for replacing the cells and tissues and use the fat and carbohydrates for energy. Kidney diets also contain a lower amount of phosphorus. Phosphorus accumulates in the blood when the kidneys are diseased. Kidney diets control the amount of other substances that may be too high or too low in patients with CKD such as salt, potassium, magnesium and B vitamins. There are differences in the kidney diets for dogs and cats. When making diet changes it is often beneficial to gradually introduce the new diet by adding increasing amounts of the new diet while reducing the amount of the current diet over 1 to 2 weeks. The pet is more likely to accept a new diet when it is introduced gradually and it is less stressful to the kidneys to gradually adapt to changes in the diet.
body weight
PCV
urine protein-to-creatinine ratio
creatinine
potassium
calcium
parathyroid hormone concentrations.
Because pets with kidney disease cannot conserve water by making concentrated urine, their water intake is very important to prevent dehydration. Make sure they always have plenty of fresh water available. If the pet is not eating well, or is vomiting, then s(he) may not be drinking enough and may get dehydrated. Pets can be encouraged to drink by giving them flavored broths in addition to plain water. The broth should be low in sodium and its best to discuss with your veterinarian other ingredients in the broth to make sure it doesn't contain substances that will make the kidneys work harder.
Lack of appetite and increased loss of potassium in urine may result in low body potassium (hypokalemia). Cats with CKD are more likely to have low body potassium than are dogs. Cats with low potassium may develop painful muscles. Both cats and dogs may be weak when potassium is low. Cat kidney diets contain higher levels of potassium so additional supplementation is probably not needed unless the cat shows signs of muscle pain. Potassium gluconate or citrate can be given by mouth if potassium supplementation is needed. Potassium chloride is acidifying and is not recommended.
Pets with CKD usually have increased blood phosphorus. In health, phosphorus and calcium are controlled by a hormone called parathyroid hormone (PTH). PTH works with vitamin D on the intestine, kidney and bone to keep calcium and phosphorus normal. As the kidneys fail the amount of PTH in the body is elevated and the amount of vitamin D is reduced. Elevated PTH itself may be responsible for some of the signs shown by pets with CKD. PTH draws calcium and phosphorus from the bones which can weaken bones which can lead to bone fracture.
Some pets with CKD will have an acid blood pH. Kidney diets are designed to counteract the acidosis but very sick animals that are hospitalized may need addition treatment to correct the acidosis.
Diseased kidneys are less efficient at regulating sodium and sodium in turn helps control blood volume and pressure. Excess sodium can lead to water retention and not enough sodium can lead to dehydration. When changing diets that contain different amounts of sodium (kidney diets usually have less sodium than regular diets) make the change gradually over several weeks. Use caution when giving your pet table scraps or treats that may be high in sodium.
Many pets with CKD have high blood pressure. High blood pressure can contribute to further decline of kidney function and can occasionally lead to sudden blindness from retinal detachment. Ideally blood pressure should be measured by your veterinarian and hypertension confirmed before giving drugs to treat high blood pressure but measuring true blood pressure in dogs and cats can be difficult. If the pet has an elevation in blood pressure it may be due to the excitement of being examined or due to CKD. The calmer you are able to keep your pet during examination, the more reliable the readings for blood pressure. There are several drugs that may be used to manage high blood pressure including enalapril, benazepril, or amlodipine (and others). Enalapril and benazepril are in a class of drugs called <align="left"> ACE inhibitors and are sometimes used in pets with CKD that have abnormal amounts of protein in their urine even when blood pressure is normal.
The kidneys play a role in producing a hormone called erythropoietin which stimulates the production of new red blood cells. Red blood cells live about a hundred days so new cells are continually being made. Less erythropoietin is made in pets with CKD leading to anemia. The packed cell volume (PVC) (also called hematocrit) is the percentage of blood cells compared to fluid in whole blood. When the PCV is ~20 in cats and ~ 25% in dogs, anemia may contribute to lack of activity and weakness.
Certain types of fats (polyunsaturated omega 6 fatty acids) may slow the decline in kidney function are are often present in kidney diets.
Some cats and dogs with kidney disease may not drink enough to prevent becoming dehydrated and may benefit from the administration of intermittent SC fluids. If your veterinarian feels your pet may benefit from giving subcutaneous fluids, we provide some instructions on how to give SC fluids. See Cat Fluids or Dog Fluids
The accumulation of wastes in the body often decreases appetite. A goal of several of the above treatments is to reduce the amount of wastes in the blood. If the pet remains off food despite above treatments you might try different brands of renal failure diets, warming the food or adding odiferous toppings to entice the pet to eat.
Increased levels of waste products cause the pet to vomit. Your veterinarian may recommend medications that reduce nausea or act directly on brain centers to reduce the urge to vomit.
Because the kidneys are responsible for elimination of many drugs, make sure that your veterinarian is aware of any other medications you are giving your pet as these may accumulate in the body to toxic levels if the kidneys cannot eliminate them.
If the urine shows signs of infection or if a urine culture grows bacteria then antibiotics may be administered. If a urinary tract infection is involving the kidneys, the period of treatment is much longer than a infection of the bladder. Avoiding Stress
Diabetes
Diabetes mellitus occurs when the pancreas doesn't produce enough insulin. Insulin is required for the body to efficiently use sugars, fats and proteins.
Diabetes most commonly occurs in middle age to older dogs and cats, but occasionally occurs in young animals. When diabetes occurs in young animals, it is often genetic and may occur in related animals. Diabetes mellitus occurs more commonly in female dogs and in male cats.
Certain conditions predispose a dog or cat to developing diabetes. Animals that are overweight or those with inflammation of the pancreas are predisposed to developing diabetes. Some drugs can interfere with insulin, leading to diabetes. Glucocorticoids, which are cortisone-type drugs, and hormones used for heat control are drugs that are most likely to cause diabetes. These are commonly used drugs and only a small percentage of animals receiving these drugs develop diabetes after long term use. The body needs insulin to use sugar, fat and protein from the diet for energy. Without insulin, sugar accumulates in the blood and spills into the urine. Sugar in the urine causes the pet to pass large amounts of urine and to drink lots of water. Levels of sugar in the brain control appetite. Without insulin, the brain becomes sugar deprived and the animal is constantly hungry, yet they may lose weight due to improper use of nutrients from the diet. Untreated diabetic pets are more likely to develop infections and commonly get bladder, kidney, or skin infections. Diabetic dogs, and rarely cats, can develop cataracts in the eyes. Cataracts are caused by the accumulation of water in the lens and can lead to blindness. Fat accumulates in the liver of animals with diabetes. Less common signs of diabetes are weakness or abnormal gait due to nerve or muscle dysfunction. There are two major forms of diabetes in the dog and cat: 1) uncomplicated diabetes and 2) diabetes with ketoacidosis. Pets with uncomplicated diabetes may have the signs just described but are not extremely ill. Diabetic pets with ketoacidosis are very ill and may be vomiting and depressed. The diagnosis of diabetes is made by finding a large increase in blood sugar and a large amount of sugar in the urine. Animals, especially cats, stressed by having a blood sample drawn, can have a temporary increase in blood sugar, but there is no sugar in the urine. A blood screen of other organs is obtained to look for changes in the liver, kidney and pancreas. A urine sample may be cultured to look for infection of the kidneys or bladder. Diabetic patients with ketoacidosis may have an elevation of waste products that are normally removed by the kidneys. The treatment is different for patients with uncomplicated diabetes and those with ketoacidosis. Ketoacidotic diabetics are treated with intravenous fluids and rapid acting insulin. This treatment is continued until the pet is no longer vomiting and is eating, then the treatment is the same as for uncomplicated diabetes. Insulin comes from different sources including beef or pork pancreas and a human genetically engineered form called Humulin. The availability of animal-source insulins continues to decline. In general, cats and small dogs need insulin injections more frequently, usually twice daily, compared to large breed dogs that may only require one dose of insulin daily. The action of insulin varies in each individual and some large dogs will need 2 insulin shots daily. The insulin needs of the individual animal are determined by collecting small amounts of blood for glucose (sugar) levels every 1-2 hours for 12-24 hours. This is called an insulin-glucose-response curve. When insulin treatment is first begun, it is often necessary to perform several insulin-glucose-response curves to determine: The animal's insulin needs may change over time requiring a change in insulin type or frequency of injection. Insulin- glucose- response curves are usually performed several days after a change in insulin is made. Before you give insulin injections to your pet, your veterinarian will show you how to: Insulin is fragile and will become less effective or even inactive, if it gets too hot or cold, or is shaken vigorously. Pay attention to the expiration date on the bottle. Discard insulin that is outdated. You may be able to practice using water and giving the "shot" to an object such as a piece of fruit until you are comfortable using needles, syringes and drawing accurate amounts of fluid into a syringe. Insulin syringes can fill to hold: Remove the syringe and needle from the outer wrapping. Do not remove the needle cap until you are ready to draw insulin into the syringe. The smallest lines between the numbers on a 100 unit syringe, measure 2 units of insulin. 30 unit syringes are numbered by 5's; 5, 10 , 15, etc. The smallest lines between the numbers on a 30 unit syringe, measure 1 unit of insulin. The insulin bottle should not be shaken but rather gently rolled between your hands to mix the insulin in the bottle. Hold the syringe between the thumb and index finger. Pull back on the plunger to the desired dose level drawing some air into the syringe. You can either pull back the plunger using the middle finger of the hand holding the syringe or... Place the needle in the center of the rubber stopper. If the needle is not centered you may be trying to force the needle through the metal ring that is holding the rubber stopper in place and will break the needle. The air is placed in the bottle so a vacuum does not form in the bottle which makes it more difficult to draw insulin from the bottle. If there is only a small amount of insulin left in the bottle, you may only be able to insert the needle into the bottle part way or else you will pass through the fluid and into the air in the bottle. Draw back on the plunger to the correct dose using your middle finger to pull back the plunger. Remove the syringe and needle from the insulin bottle. Holding the syringe with the needle pointed up, gently "flick" the syringe to get the air to rise to the top. Usually the skin is not cleansed before inserting the needle. If the cat has a normal immune system, the few bacteria that are pushed under the skin with the needle will be killed by the cat's immune system. You can use alcohol on a cotton ball to make the hair lay flat so it is easier to see where the hair ends and the skin starts. Alcohol takes about 30 minutes before bacteria are killed, so just swiping the hair with alcohol is not effective in killing bacteria. If you get neither air nor blood, the needle is placed correctly and you can push the plunger to inject the insulin. Give the insulin shots in different locations each time. Syringes and needles used to give insulin should not be discarded in the trash but should be placed in a puncture-proof container and taken to your veterinarian for disposal. Insulin injections are not as perfect as the insulin produced by the pancreas. Blood sugar levels will not always be normal in diabetic pets. The goal of treatment is to reduce the signs of diabetes. When diabetes is well controlled with insulin, the pet should drink, eat and urinate normal amounts. They should have a good appetite, without becoming fat and should have normal activity. Insulin needs are closely related to the type of food eaten by the pet. Your veterinarian will recommend a specific diet and feeding regimen that will enhance the effectiveness of insulin. If your pet is overweight, s(he) will be placed on a weight-reducing diet. As the pet loses weight, less insulin will be needed. Only feed the recommended diet..NO table scraps or treats that are not part of the recommended diet. Heavy exercise will reduce the amount of insulin needed. It is important to talk to your veterinarian before making changes in diet or exercise. There is always some risk that a diabetic patient will develop low blood sugar. Signs of low blood sugar include weakness, staggering, seizures, or just being more quiet than usual. You should keep corn syrup on hand to rub on the animals gums if they have signs suggestive of low blood sugar. Don't pour large amounts of corn syrup in the mouth of an animal that is not fully conscious as the syrup may be inhaled into the lungs. Because insulin needs vary with the activity and lifestyle of your pet, you may want to keep a written daily log of: Your veterinarian may ask you to check your pet's urine for sugar using a test strip. If your pet is well regulated on insulin, the sugar readings in most urine samples will be negative or trace. The strips may have color pads only for glucose or for glucose and ketones. The strip is placed in fresh urine and the color change compared with the colors on the bottle. Be sure to follow the label instructions for timing when to read the results. You should never change the dose of insulin based on the urine sugar reading alone. Animals can have lots of sugar in their urine either when the insulin dose is too low or is too high. There are many styles of machines used to measure blood sugar. The machines are called glucometers. They use color sticks which are read by the glucometer rather than by color changes you can see. Different styles of glucometers use different color strips. Diabetes is rarely reversible in dogs, but diabetic cats will sometimes regain the ability to produce their own insulin in the pancreas. Cats that developed diabetes after receiving long term glucocorticoids or hormones are more likely to stop needing insulin after a while compared to cats that developed diabetes without a known cause. You should have your diabetic pet evaluated by a veterinarian at 2-4 month intervals or anytime another health problem develops. The development of other health problems will often interfere with insulin regulation.
Diabetes is managed long term by the injection of insulin by the owner once or twice a day. Some diabetic cats can be treated with oral medications instead of insulin injections, but the oral medications are rarely effective in the dog. There are three general types of insulin used in dogs and cats:
Not all syringes used to inject insulin are alike. When you buy additional supplies, make sure that you buy the right kind of syringes. Insulin needles are very thin to reduce discomfort during injection.
The syringe is packaged in sterile paper or plastic wrapping or in a plastic case. The needle is covered with a plastic cap to keep it sterile. Use a new syringe-needle combination for each injection.
Insulin syringes have the needle attached. The needle is covered with a plastic cap to prevent the needle from puncturing the wrapping and to keep the needle from bending or breaking.
The plunger fits inside the hollow barrel of the syringe and is pulled part way out of the barrel to draw insulin into the syringe. The plunger is pushed into the barrel of the syringe to push insulin through the needle. The finger grip makes it easier to hold the syringe.
100 unit syringes are numbered by 10's; 10, 20, 30, etc.
The position of the TOP of the black rubber stopper on the plunger is used to measure the volume of insulin in the syringe. The TOP of the black rubber stopper is the part closest to the needle.
Before each injection,
Remove the plastic cap from the needle.
Hold the syringe in your left hand between the thumb and index finger and use the thumb and index finger of the other hand to pull the plunger or...
Place your index finger against the finger grip and pull the plunger with your thumb and middle fingers.
Hold the insulin bottle upside down in your left hand if you are right handed (opposite for left-handed individuals).
Use your thumb to push the plunger and inject the air into the bottle.
Insert the entire length of the needle into the insulin bottle as long as the tip of the needle is in the fluid in the bottle. Insulin needles are very thin and easily bent. You are less likely to bend the needle while drawing insulin into the syringe, if the needle is inserted all the way into the bottle.
If it is difficult for you to pull the plunger with your middle finger, you can use the thumb and index finger to pull the plunger. So that you do not pull the needle out of the bottle, curl the three fingers of your right hand that are not holding the bottle around the syringe trapping it against your palm. Then pull the plunger with the thumb and index finger. Your fingers may be covering the numbers on the syringe so draw more than you need, then push the extra back into the bottle, until the correct amount remains in the syringe.
...or place your index finger against the finger grip to keep the needle from pulling out of the bottle and pull the plunger with your thumb and middle fingers.
If there is an air bubble in the syringe, draw a little more insulin than the correct dose.
Press the plunger with your thumb to push the air out of the syringe, until the correct amount of insulin remains in the syringe.
This 30 unit syringe has been filled to 14.5 units.
There is 1 unit between each back line on this smaller syringe. Smaller syringes allow for more accurate measurements of small amounts of insulin. The top of the black rubber stopper is half way between 14 and 15 units.
This 100 unit syringe has been filled to 48 units. There are 2 units between each black line on the barrel. The volume is measured at the TOP of the black rubber stopper on the plunger.
Pinch up a fold of skin anywhere along the neck or back using your left hand if you are right-handed. Use your right hand to place the needle into the skin fold along the long axis of the fold.
If you place the needle in the opposite direction, across the skin fold, it is more likely that the needle will go through one fold of skin and out the other fold of skin, or may poke into your finger.
Pull back the plunger. If you get air, you placed the needle through both folds of skin. Remove the needle and try again. If you get blood, the tip of the needle is in a blood vessel. Remove the needle and try again.
The top color pad is to read urine sugar. This sample is negative for sugar. The bottom color pad is for ketones and is also negative for ketones.
The glucose pad has turned brown indicating a large amount (>2000mg/dl) of sugar in the urine. The urine is negative for ketones.
If your pet is difficult to regulate with the proper dose of insulin you may be taught how to take a small blood sample from your pet to measure blood sugar readings at home.
Diarrhea
Diarrhea is the passing of loose or liquid stool, more often than normal. Diarrhea can be caused by diseases of the small intestine, large intestine or by diseases of organs other than the intestinal tract. Your ability to answer questions about your pet's diet, habits, environment and specific details about the diarrhea can help the veterinarian narrow the list of possible causes, and to plan for specific tests to determine the cause of diarrhea. (Anatomy of the digestive system: dog / cat)
Small intestinal and large intestinal diarrhea have different causes, require different tests to diagnose and are treated differently. Small intestinal diseases result in a larger amount of stool passed with a mild increase in frequency; about 3 to 5 bowel movements per day. The pet doesn't strain or have difficulty passing stool. Animals with small intestinal disease may also vomit and lose weight. Excess gas production is sometimes seen and you may hear the rumbling of gas in the belly. If there is blood in the stool it is digested and black in color. Disease of the large intestine including the colon and rectum cause the pet to pass small amounts of loose stool very often, usually more than 5 times daily. The pet strains to pass stool. If there is blood in the stool, it is red in color. The stool may be slimy with mucus. The pet does not usually vomit or lose weight with large bowel diarrhea. A sudden onset of small intestinal diarrhea may be caused by viruses including canine distemper, canine parvovirus, canine coronavirus, feline panleukopenia virus or feline coronavirus, in young, poorly vaccinated pets. Small intestinal diarrhea can be caused by bacteria such as salmonella, clostridia or campylobacter although these same bacteria can be found in the stool of normal dogs and cats. Worms and giardia can cause small intestinal diarrhea, mostly in young animals. Foreign bodies including bones, sticks and other objects can pass through the stomach and get stuck in the intestine causing both diarrhea and vomiting. These same foreign materials may pass through the intestinal tract without getting stuck but may damage the lining of the intestinal tract causing diarrhea. Dietary indiscretion or a sudden change in diet can cause diarrhea with or without vomiting. Food allergies in dogs and cats can cause diarrhea, vomiting or itchy skin. Toxins including lead and insecticides can cause diarrhea usually with vomiting. Inflammatory bowel disease (IBD) occurs commonly in both dogs and cats. In IBD the walls of the intestine contain abnormal numbers of inflammatory cells which can be eosinophils, lymphocytes or plasma cells. The cause of IBD is not known but is suspected to be an allergic reaction to components of food, bacteria or parasites. IBD can be congenital in some breeds of dogs, for example Basenji dogs may develop a severe inflammatory bowel disease. Tumors of the intestine are another cause of diarrhea usually occurring in older pets. The tumor may be a single mass when the tumor is from the glands of the intestine (adenocarcinoma) and may be removed by surgery or the tumor may occur diffusely along the intestine. Lymphosarcoma occurs in both dogs and cats and can either be a single or multiple masses in the intestine or the abnormal lymphocytes may be spread through out the intestine. Lymphosarcoma is often responsive to anti-cancer drugs in cats but rarely responds to anti-cancer drugs in dogs. In certain parts of the country small intestinal disease can be caused by fungal infections including histoplasmosis. Your veterinarian can discuss with you whether histoplasmosis is seen in your part of the country. Diseases outside the intestinal tract that may cause diarrhea include kidney failure, liver failure, pancreatic disease and hyperthyroidism in the cat. Severe inflammation of the pancreas (pancreatitis) can lead to damage of the pancreas and an inability to make enough enzymes to digest fat. This is called pancreatic insufficiency and causes diarrhea with a large volume of greasy stool. Pancreatic insufficiency can occur in young animals due to a congenital deficiency of pancreatic enzymes. The cause of small intestinal diarrhea may be determined from blood tests, examination of the stool, x-rays or ultrasound of the abdomen or by endoscopy. Endoscopy is the technique of passing a flexible scope through the stomach into the upper intestine. Small biopsies of the lining of the intestine can be taken for microscopic evaluation. Endoscopy requires general anesthesia. A diagnosis of intestinal lymphosarcoma may be missed on endoscopy as the biopsies taken using endoscopy do not include the full thickness of the wall of the intestine and the cancerous cells may be deep in the wall of the intestine. A diagnosis in that case requires surgery in order to take a larger biopsy of the entire thickness of the intestine. Dogs and cats with chronic small intestinal diarrhea will lose weight as they are unable to properly absorb nutrients and may develop edema of the legs or fluid accumulation in the belly or chest. A small protein, albumin may be lost in diarrhea. Albumin acts like a sponge to keep water in the blood vessels. When albumin is lost in the stool, blood albumin gets low and water leaks out of blood vessels to accumulate in other locations. Chronic diarrhea may cause the fur to look dull and brittle due to nutrient deficiencies. Acute small intestinal diarrhea can be managed by withholding food, but not water for 24 - 48 hours. If diarrhea stops, small amounts of a bland low-fat food are fed 3 to 6 times daily for a few days, with a gradual increase in the amount fed and a gradual transition to the pet's normal diet. Foods designed as intestinal diets usually contain rice as rice is more digestible than other grains. You are discouraged from administering over-the-counter diarrhea medications without first consulting a veterinarian. If the pet is active, not dehydrated and has been previously healthy, acute diarrhea can often be managed at home. Diarrhea that continues for more than a few days or is accompanied by depression or other signs is an indication to take your pet to a veterinarian. Diarrhea of large intestinal origin can be caused by whipworms, polyps, inflammatory bowel disease, colonic ulcers or colonic cancer. Stress can cause large bowel diarrhea in excitable dogs. The diagnosis of large intestinal diarrhea is also made by blood tests and examination of the stool. A rectal examination using a gloved finger may provide some information about the cause of large bowel problems including rectal polyps and rectal cancer. Endoscopy to examine the large intestine is performed using a rigid or flexible scope passed up the rectum. Because the rectum is often very irritated, colon exams are usually performed under general anesthesia. The treatment of large bowel diarrhea may be based on a specific diagnosis. Non specific treatment of large bowel diarrhea often includes a high fiber diet and sullfasalazine, an anti-inflammatory drug. Black Earth Veterinary Clinic assumes no liability for injury to you or your pet incurred by following these descriptions or procedures.
Hypertrophic Cardiomyopathy (HCM)
Anatomy of the heart of a cat
HCM is a disease that causes thickening of the heart muscle resulting in poor relaxing and filling ability. As the heart’s pumping chamber (ventricle) becomes progressively thicker, less blood can enter the chamber; thus, less blood is ejected out to the body. The cause of HCM is unknown, although certain breeds of cats appear to be predisposed. Middle-aged male cats may be more commonly affected. Sometimes heart muscle thickening similar to HCM can develop secondary to other disorders such as hyperthyroidism (elevated thyroid hormone) and systemic hypertension (elevated blood pressure). Blood pressure measurement and, in cats over five years of age, a blood thyroid hormone test should be done to exclude these secondary causes when cardiac hypertrophy (thickening) is diagnosed.
Some pets show no sign of illness, especially early in the disease. In other cases, signs of left-sided congestive heart failure (fluid accumulation in the lung) may occur. These signs include lethargy, decreased activity level, rapid and/or labored breathing and possibly open mouth breathing with excitement or exercise. Sometimes left and right-sided congestive heart failure develop with fluid accumulation inside the chest or abdominal cavity causing greater respiratory (breathing) effort and abdominal distention. Once fluid accumulations have occurred, clinical heart failure is present and aggressive medical therapy should be sought. Other signs of this disease can include sudden weakness, collapsing episodes, and unfortunately even sudden death due to disturbances in heart rhythm. In some cats with a very large heart chamber (i.e. left atrium) a blood clot may form and if it enters the circulation may cause weakness or paralysis (usually of the rear legs). If this occurs, contact your veterinarian right away to determine if complications related to heart disease (or another disease) are present. A physical examination performed by your veterinarian may reveal a heart murmur, abnormal heart sounds, abnormal lung sounds, or irregularities in heart rhythm. Chest radiographs (x-rays), an electrocardiogram (ECG..sometimes called an EKG), and an echocardiogram (heart ultrasound) are tests often utilized to confirm a suspected diagnosis and to determine severity. A routine physical exam and one or more of these tests may be recommended every six months to one year to look for any progression of disease in cats without clinical signs. Asymptomatic pets may not need medical therapy depending on the findings of the tests listed above, but routine reevaluations will often be recommended. Other cats will need medications to slow the heart rate, and promote relaxation of the pumping chambers (ventricles). If arrhythmias or congestive heart failure signs are present, additional medications used may be required. Since this disease can be progressive, the number and the amount of medications used may change with time. Therapy is always tailored to the needs of the individual patient. If congestive heart failure is present, dietary salt reduction is also recommended. Medications commonly used for HCM: Beta-adrenergic blockers such as atenolol (Tenormin) or propanolol (Inderal). These medications slow the heart rate, which enhances filling and relaxation of the pumping chambers. Beta-blockers also allow more time for blood flow to the heart muscle itself, and reduce the amount of oxygen used by the heart. In some cases, the incidence of arrhythmias is also lessened. Side effects may include bronchospasm (spasm of the airways) (propranolol), fatigue, and in excessive doses, slow heart rate and low blood pressure. Calcium-channel blockers such as diltiazem (Cardizem CD, Dilacor XR). This class of drug has similar actions to the beta-blockers. Some differing characteristics of the calcium-blockers include little or no anti-arrhythmic activity in some cases, possible a greater ventricular relaxing effect, and a greater propensity for low blood pressure at higher doses. Other medications may be prescribed in some patients. Diuretics (furosemide, spironolactone, etc.) may be needed to control edema and effusions (congestive heart failure). In pets that have had or may be prone to blood clot formation, anti-coagulants such as aspirin, warfarin, or heparin may be prescribed. Medical therapy is always chosen to meet the needs of the individual patient. Frequent recheck examinations and adjustments may be needed especially early in the course of treatment to individualize a medication regimen. This Pet Health Topic was written by O. L. Nelson, DVM, MS, Diplomate ACVIM (Cardiology & Internal Medicine) Washington State University.
Dilated Cardiomyopathy (DCM)
What is it?
DCM is a disease of the heart muscle that results in weakened contractions and poor pumping ability. As the disease progresses the heart chambers become enlarged, one or more valves may leak, and signs of congestive heart failure develop. The cause of DCM is unclear in most cases, but certain breeds appear to have an inherited predisposition. Large breeds of dogs are most often affected, although DCM also occurs in some smaller breeds such as cocker spaniels. Occasionally, DCM-like heart muscle dysfunction develops secondary to an identifiable cause such as a toxin or an infection. In contrast to people, heart muscle dysfunction in dogs and cats is almost never the result of chronic coronary artery disease ("heart attacks").
What are the signs of this disease? Early in the disease process there may be no clinical sign detectable, or the pet may show reduced exercise tolerance. In some cases, a heart murmur (usually soft), other abnormal heart sounds, and/or irregular heart rhythm is detected by your veterinarian on physical examination. Such findings are more likely as the disease progresses. As the heart’s pumping ability worsens, blood pressure starts to increase in the veins behind one or both sides of the heart. Lung (pulmonary) congestion and fluid accumulation (edema) often develop behind the left ventricle/atrium. Fluid also may accumulate in the abdomen (ascites) or around the lungs (pleural effusion) if the right side of the heart is also diseased. When congestion, edema and/or effusions occur, heart failure is present. Weakness, fainting episodes, and unfortunately, even sudden death can result from heart rhythm disturbances (even without "heart failure" signs). What are the signs of heart failure? Dogs with heart failure caused by DCM often show signs of left-sided congestive failure. These include reduced exercise ability and tiring quickly, increased breathing rate or effort for the level of their activity excess panting, and cough (especially with activity). Sometimes the cough seems soft, like the dog is clearing its throat. Poor heart pumping ability and arrhythmias can cause episodes of sudden weakness, fainting, or sudden death as noted above. Some dogs with DCM experience abdominal enlargement or heavy breathing because of fluid accumulation in the abdomen or chest, respectively. Presence of any of these signs should prompt a visit to your veterinarian to determine if heart failure (or another disease) has developed. More advanced signs of heart failure could include labored breathing, reluctance to lie down, inability to rest comfortably, worsened cough, reduced activity, loss of appetite, and collapse. A veterinarian should be consulted right away if these signs occur. Signs of severe heart failure may seem to develop quickly with DCM, but the development of underlying heart muscle abnormalities and progression to overt heart failure probably takes months to years. How is this disease diagnosed? A cardiac exam by a veterinarian can detect abnormal heart sounds (when present) and many signs of heart failure. Usually chest radiographs (x-rays), an electrocardiogram (ECG), and echocardiogram are performed to confirm a suspected diagnosis and to assess severity. Echocardiography also can be used to screen for early DCM in breeds with a higher incidence of the disease. Resting and 24-hour (Holter) ECGs are sometimes used as screening tests for the frequent arrhythmias that usually accompany DCM in some breeds, especially boxers and Doberman pinchers. What can be done if my pet has this disease? Asymptomatic (subclinical) cases of DCM may be treated with enalapril or another ACE inhibitor to slow progression of the changes leading to heart failure. Other medications and strategies are also used as signs of heart failure develop and/or if rhythm abnormalities are present. Therapy is always tailored to the needs of the individual patient. Since this disease is not reversible and heart failure tends to be progressive, the intensity of therapy (for example, the number of medicines and the dosages used) usually must be increase over time. This Pet Health Topic was written by O. L. Nelson, DVM, MS, Diplomate ACVIM (Cardiology & Internal Medicine) Washington State University.
Heart Valve Malfunction in the Dog (Mitral Insufficiency)
Many dogs slowly develop degenerative thickening and progressive deformity of one or more heart valves as they age. In time, these changes cause the valve to leak. The mitral valve is most commonly affected. This valve separates the blood collecting chamber (left atrium) from the pumping chamber (left ventricle) leading to the body. Some dogs also develop these changes in the tricuspid valve, which separates the collecting (right atrium) and pumping (right ventricle) chamber leading to the lungs.
Certain breeds have an inherited predisposition to this disease. Degenerative valvular disease is slowly progressive over years and is non-reversible. The volume of blood that leaks back into the atrium with each heartbeat tends to increase slowly over time. However, many dogs with this disease never develop signs of congestive heart failure even though they may have a loud murmur. Early in the disease process, your veterinarian may hear a soft murmur when the affected valve starts to leak. There usually is no noticeable change in the dog’s activity level or behavior for a long period of time. Gradually, though, the valve leak tends to get worse and the heart slowly enlarges. If the leak becomes severe, blood may start to back up behind the heart – usually into the lungs. This causes lung congestion and fluid accumulation (edema). When lung congestion and edema occur, congestive heart failure is present. Reduced exercise ability may be the first sign of heart failure. Most dogs with heart failure caused by degenerative valve disease show signs of "left-sided" congestive failure. These signs include tiring quickly, increased breathing rate or effort for the level of activity, excessive panting, and cough (especially with activity). The presence of any of these signs should prompt a visit to your veterinarian to determine if heart failure (or another disease) has developed. More advanced signs of heart failure could include labored breathing, reluctance to lie down, inability to rest comfortably, worsened cough, reduced activity, and loss of appetite. Your veterinarian should be consulted right away if these signs occur. Some dogs that become symptomatic from their heart disease develop fluid in the abdomen (ascites); others have episodes of sudden weakness or fainting that can result from irregular heartbeats or other complications. As long as no sign of heart failure develops, no treatment is necessary, although reduction of dietary salt intake is often advised. Again, there are many dogs with degenerative valvular disease that never progress to heart failure. However, if heart failure develops, several medications and other strategies are used to control the signs. Since the disease is not reversible and heart failure, when it occurs, tends to be progressive, the intensity of the therapy (including the number of medicines and dosages used) usually must be increased over time. Therapy is always tailored to the needs of the individual patient. This Pet Health Topic was written by O. L. Nelson, DVM, MS, Diplomate ACVIM (Cardiology & Internal Medicine) Washington State University.
Holiday Health Hazards
If you want to get festive, mix some of your pet's regular food with water to make a "dough" and roll out and cut into festive shapes, then bake until crunchy.
The holiday season brings excitement and commotion associated with shopping, final exams, travel, and other seasonal preparations. In all the activities of the season our beloved pets may be exposed to hazards less commonly found other times of the year. As homes fill with holiday spirit, pets may be intrigued by the new sites, smells and tastes. The following are some of the most common health concerns for your pet during the holidays. If you have specific questions regarding any pet health concern please contact your veterinarian.
Tinsel, Ribbon and other Pretty Things Ribbons, wrapping paper, ornaments, tinsel, extension cords and gifts may be appealing "chew toys" that may make your pet sick. There is something about those shiny strands of Christmas tree decor, which drives kitties wild. Although the sight of your cat pawing at the tree may be cute, the ingestion of tinsel can be deadly. Eating tinsel or other string-like items such as ribbon (often called linear foreign bodies) can cause serious damage to the intestine. One end can get stuck while the rest is pulled into the intestine as it contracts; the contractions may cause the ribbon or tinsel to saw through the intestine. If not caught in time, infection of the belly cavity develops and the prognosis for recovery becomes poor. Pets with linear foreign bodies quickly become ill with signs including vomiting, diarrhea, depression, belly pain and sometimes fever. Eating other holiday decorations can cause signs ranging from mild depression to severe vomiting or diarrhea, depending upon whether or not the foreign matter can be passed in the stool or gets stuck along the way. Foreign matter stuck in the intestine often does NOT show up on "x-ray" but sometimes the foreign matter will trap air in the intestine, which helps your veterinarian make a diagnosis. Surgery is required to remove foreign matter that does not pass out on its own. Holiday Lights Decorative lights are another attraction for pets to chew on. Both indoor and outdoor lights should be carefully examined to ensure safety for your household pets. Electrical shock may occur from defective cords as well as from pets chewing on cords. Check cords for any signs of bite marks, loose or frayed wires, proximity to the tree's water supply or evidence of short circuits. Use grounded "3-prong" extension cords and strictly follow manufacturer's guidelines for light usage. Electrical shock can cause burns, difficulty breathing, abnormal heart rhythm, loss of consciousness, and death. Call a veterinarian immediately if your pet has been injured by electrical shock. Treatment will be most effective if begun soon after the shock. Water, Water... Even though they have their own water bowel, there is something enticing about a novel source of water; whether it's the toilet bowl or the Christmas tree stand. If you add chemicals to the water meant to keep your tree fresh longer, be sure to read the label to make sure it is safe for pets. Potpourri makes your house smell festive but may be another attraction for pets to drink. Make sure that potpourri pots are covered or otherwise inaccessible to pets. It may be difficult to curb your pet's fascination with all those pretty decorations. Child gates can be used across doorways to keep your pet away from the Christmas tree and decorations at times they cannot be watched. Overindulgence Well-intentioned family and friends may share holiday foods with pets causing the pet to develop a stomach upset or worse, pancreatitis (inflammation of the pancreas) which can be caused by eating fatty foods. To control excessive food intake by your pets and meet your guests' desires to feed the pets, dole out the treats your pets would normally receive and let your guests "treat" the pets. If you want to get festive, mix some of your pet's regular food with water to make a "dough" and roll out and cut into festive shapes, then bake until crunchy. Extra attention from visiting relatives and friends may be relished by some pets while others seek solitude in their favorite hiding spot. Make sure pets are given some "personal space" if they want to get away from the commotion. Some pets may respond to all the hullabaloo with a change in behavior including bad behaviors like eliminating in the house. Try to spend a little extra "quality time" with your pet to assure them they have not been forgotten. Chocolate What would the holidays be without boxes of chocolate and warm cocoa in front of the fire? However, chocolate can be toxic or even fatal to dogs and cats. Chocolate may be mistakenly given to pets as treats and may be irresistible to the curious canine. Chocolate poisoning occurs most frequently in dogs but other species are also susceptible. Theobromine is the toxic compound found in chocolate. Signs which may appear within 1 to 4 hours of eating chocolate include: The toxicity of chocolate depends on the amount and type of chocolate ingested: The amount of theobromine in white chocolate or chocolate flavored dog treats is usually negligible. As with any poisoning, call your veterinarian or an emergency veterinary hospital immediately if you suspect your pet may have ingested chocolate. Have the product label information available when you call your veterinarian. There are national and regional poison control hotlines for animals. In general, the treatment of poisonings is most effective if begun soon after eating the poison, before large amounts are absorbed into the blood. Poinsettias & Mistletoe Mistletoe can be very toxic to animals and you should seek veterinary consultation immediately if your pet has potentially ingested any part of the plant. Mistletoe can cause vomiting, severe diarrhea, difficult breathing, shock and death within hours of ingestion. Pets as Gifts A cute, cuddly puppy or kitten may seem to be the perfect gift but unfortunately after the holiday season the population of animal shelters explodes with these "surprise gifts". Owning a pet is a long-term commitment that not every one can make. Dealing With Death or Severe Illness over the Holidays The holiday season heightens our emotions and can be a very difficult time to deal with the loss or illness of a companion animal. The bond between animals and humans is often very strong and losses can be very painful. If you or someone you know needs support without judgment from those who appreciate your feelings and may be able to help, please contact the WSU College of Veterinary Medicine Pet Loss Hotline. From all of us at the College of Veterinary Medicine at WSU, best wishes for a safe and happy holiday season for you and your pets. Other Holiday & Seasonal Tips: Gifts for the Pet Owner and other Holiday Tips Prevention of Antifreeze Poisoning This Pet Health Topic was written by Paul Chauvin, Washington State University, Class of 2004.
Source
Potential Toxic Dose (44lb dog)
Unsweetened Cocoa
3oz
Baking Chocolate
5oz
Semisweet Chocolate
7oz
Milk Chocolate
20oz
 Poinsettias fill homes with color during the holidays. Poinsettias have received bad publicity in the past whereas in fact, poinsettias are not very toxic to pets. They do contain a milky sap that can irritate the mouth but if signs develop they are usually mild.
Poinsettias fill homes with color during the holidays. Poinsettias have received bad publicity in the past whereas in fact, poinsettias are not very toxic to pets. They do contain a milky sap that can irritate the mouth but if signs develop they are usually mild. There are many species of Holly (genus Ilex) Berries and leaves can be a problem although signs of poisonings are generally mild, and include vomiting, belly pain, and diarrhea.
There are many species of Holly (genus Ilex) Berries and leaves can be a problem although signs of poisonings are generally mild, and include vomiting, belly pain, and diarrhea.
Hyperthyroidism in the Cat
Hyperthyroidism is the overproduction of thyroid hormone by the thyroid glands. Hyperthyroidism occurs most commonly in older cats and is rare in dogs. The average age of cats with hyperthyroidism is 13 years of age; only about 5 % of hyperthyroid cats are younger than 10 years of age. There are 2 thyroid glands located in the neck. One or both of the glands can enlarge and overproduce thyroid hormone. Involvement of both glands is more common than involvement of one gland. Thyroid hormone affects the function of most organs in the body, so the signs of hyperthyroidism are quite variable.
Signs of hyperthyroidism can include: A diagnosis of hyperthyroidism is made when the level of thyroid hormone is increased in the blood. Most hyperthyroid cats have very high levels of hormone but some cats will have signs of hyperthyroidism with normal or only slightly increased levels of thyroid hormone. Thyroid hormone levels can vary over time so it may be necessary to check blood levels several times or perform a different test called a T3 suppression test. The enlarged thyroid gland(s) can often be felt in the neck. If the diagnosis is not obvious by blood tests, a nuclear medicine scan of the thyroid glands can be performed at certain specialty veterinary practices. The cat is given a small dose of a radioactive compound that travels by the blood to the thyroid glands. Hyperactive thyroid glands accumulate more of the compound than normal glands. After this test the cat must be hospitalized for a few days while it clears the radioactive compound from its body. A blood panel and urinalysis are also performed to screen for abnormalities in other organs such as liver and kidney that may be present due to the advanced age of the animal. High levels of thyroid hormone may cause heart disease. The heart may appear enlarged on x-ray or ultrasound and may show abnormal electrical activity on an ECG (electrocardiogram). Heart disease may cause fluid to build up in or around the lungs. Cats with serious heart disease and hyperthyroidism need to be treated for both diseases. The heart disease will reverse in many cats after successful treatment of hyperthyroidism. There are three types of treatment for hyperthyroidism: All three treatments will reduce thyroid hormone levels and the signs of hyperthyroidism. Discuss the 3 options with your veterinarian. If your pet has other diseases, one treatment may be better for your cat than another. The anti-thyroid pill is methimazole, also known as Tapazole. Methimazole is given one to three times daily and must be continued life long. It takes several weeks for methimazole to reduce blood thyroid hormone levels to normal. If methimazole is discontinued, thyroid hormone levels will return to high levels over a few weeks. Methimazole may be used to reduce thyroid hormone levels to normal before surgically removing the thyroid gland(s). Cats with heart disease may be too sick and fragile to anesthetize for surgery in which case methimazole can be given until the heart improves and the cat is stronger. Some owners (and their cats) find it difficult to give pills daily and may decide, after starting anti-thyroid pills, to later have their cat treated with radioactive iodine or surgery. Methimazole may produce side effects in cats including depression, vomiting and lack of appetite. These signs usually resolve without stopping the medication. A more serious side effect is the development of low blood cell counts which are more likely to develop during the first 3 months of treatment. Blood cell counts should be evaluated every 2 weeks during the first 3 months. If blood cell counts decrease methimazole is stopped and another treatment method should be considered. Enlarged thyroid glands can be surgically removed. Methimazole is given for 1 to 2 months before surgery so that thyroid hormone levels are normal at the time of surgery. If both glands are enlarged, they can both be removed and most cats will still produce enough thyroid hormone by a few thyroid cells scattered through out the body to prevent hypothyroidism (abnormally low thyroid hormone levels). A few cats will become hypothyroid and may need to take thyroid pills. Surgical removal of the thyroid gland(s) can usually be performed without complications. Occasionally complications may develop including damage to the parathyroid glands, which are closely attached to the thyroid gland, damage to nerves close to the thyroid gland or damage to the voice box. Parathyroid gland damage causes low blood calcium that may cause seizures. Low blood calcium is treated with calcium or vitamin D. Nerve damage causes abnormal size of the pupils of the eyes and droopy eyelids. Damage to the voice box causes a change in voice. Some cats will remain hyperthyroid after surgical removal of the thyroid glands. These cats have thyroid cells in abnormal locations, including inside the chest cavity where surgical removal is difficult. This extra thyroid tissue is called ectopic thyroid. If you and your veterinarian decide that surgery is the best treatment option for your cat, a nuclear medicine scan (described in the diagnosis section) could be performed at a specialty veterinary practice before surgery to see if your cat has ectopic thyroid tissue. If ectopic thyroid tissue is seen on the nuclear medicine scan, then a different treatment, either methimazole or radioactive thyroid treatment should be selected. Cats that have had surgery may have recurrence of hyperthyroidism. Blood thyroid hormone levels should be measured once or twice a year. Treatment with radioactive iodine is only performed at selected specialty veterinary practices. Radioactive iodine is given intravenously and will accumulate in the abnormal thyroid tissue killing the abnormal thyroid cells but sparing the normal thyroid cells. Radioactive iodine will also accumulate in ectopic thyroid tissue. Radioactive iodine treatment is very effective and rarely causes hypothyroidism. The cats do not have to be placed under anesthesia for the procedure. The disadvantages of radioactive iodine treatment include the need to travel to a facility that offers this treatment and the need for the cat to remain hospitalized until the level of radioactivity decreases to a safe level as determined by the state radiation control office (usually 1 to 3 weeks). Radioactive iodine treatment of hyperthyroid cats is available at Washington State University. Older cats with hyperthyroidism often also have kidney disease. Treatment of these cats is a delicate balancing act. Hyperthyroidism can actually improve kidney function by increasing blood flow to the kidneys. Some cats with kidney disease will show a worsening of kidney function after treatment for hyperthyroidism. Talk to your veterinarian about monitoring kidney function in hyperthyroid cats.
A nuclear medicine scan of the thyroid glands.
Both thyroid glands are abnormal in this cat and take up the radioactive compound. The other black spot is the stomach lining which will also take up the compound.
Hypothyroidism in Dogs
The thyroid glands located in the neck produce hormones that affect the function of many parts of the body. Although thyroid disease in cats often causes over productive glands and too much hormone, dogs with thyroid disease usually have a low production of thyroid hormones.
Overactive thyroid glands in the dog are rare and are usually associated with cancer. Hypothyroidism in dogs is usually caused by inflammation or shrinkage of the thyroid gland. Thyroid cancer can cause hypothyroidism although it does not occur commonly in dogs. Hypothyroidism occurs more commonly in medium to large breed dogs and usually in middle aged dogs. Breeds commonly affected include:
- Golden retriever
- Doberman pincher
- Irish setter
The most common signs of low thyroid function in dogs include loss or thinning of the fur, dull hair coat, excess shedding or scaling, weight gain, reduced activity and reduced ability to tolerate the cold. The hair loss occurs primarily over the body, sparing the head and legs, and is usually not accompanied by itching or redness of the skin. Some dogs will have thickening of the skin and increased skin pigment, especially in areas of friction, such as the armpit (axilla). Hypothyroid dogs often have ear infections and show ear pain, redness, and odor. Hypothyroid dogs may also develop skin infections which may be itchy and result in sores on the body. The accumulation of substances called mucopolysaccharides can cause the muscles of the face to droop giving the dog a facial expression that is sometimes called “tragic”. Less commonly recognized signs that may be seen in a small number of dogs with hypothyroidism include dilation of the esophagus (megaesophagus) causing regurgitation, and abnormal function of nerves or muscles leading to weakness or abnormal ability to walk. Routine blood tests can be affected by hypothyroidism, although the changes are not consistent and can be subtle. Dogs may have a mild anemia and increased levels of cholesterol. There are several blood tests that can be used to confirm a suspected diagnosis of hypothyroidism. Blood testing for hypothyroidism is often performed as a panel of several tests in order to increase the yield of these tests. The results of some of these tests can be influenced by the presence of other non-thyroid diseases, so test results must be considered in light of the whole picture. Treatment of hypothyroidism is by giving oral replacement hormone for the rest of the dog’s life. Initially thyroid hormone is usually given twice daily. Once the hair coat begins to improve, some dogs can be maintained on once daily medication. There are two general forms of thyroid medication, T3 and T4. T4 is converted to T3 by the body. Most hypothyroid dogs given T4 will convert it to T3 so almost all hypothyroid dogs receive T4 (levothyroxine or L-thyroxine). A few dogs are unable to make this conversion and require T3 medication. It usually takes 4 to 6 weeks before regrowth of the fur is apparent. In dogs with associated ear infection, the ears should be cleaned and treated with antibiotics either in the ear or by mouth. Blood levels of the T4 are often measured in order to fine tune the dose.
Urinary Incontinence
Urinary incontinence is the involuntary passing of urine. Pets can be incontinent for many different reasons. Those reasons can involve the bladder, the urethra which is the tube from the bladder to the outside, or incontinence can be caused by abnormalities in the parts of the brain and spinal cord that control bladder function. Related anatomy dog/ cat
Incontinence can be confused with diseases that cause a pet to urinate frequently. This pet health topic only discusses incontinence, not frequent urination.
Incontinence can also be confused with submissive urination. Submissive urination occurs when a dog is acting submissive to a person or to another dog. Submissive urination occurs more frequently in young animals. The dog usually rolls on its back and urinates. These dogs can also urinate normally. Young animals may have a birth defect causing incontinence. The most common birth defect that causes incontinence in young dogs is ectopic ureter(s). The ureters carry urine from the kidneys to the bladder. If one or both ureters by-pass the bladder and connect to an abnormal location such as the urethra or vagina, the puppy may drip urine. Siberian Huskies are most often affected. Other breeds that have a higher occurrence of this birth defect include: Female dogs are more commonly affected. If only one ureter is abnormal the dog will dribble urine but can also urinate normally. If both ureters are affected then the puppy will only dribble urine and cannot pass urine normally. To diagnose this condition a dye study of the bladder is usually performed. Sometimes the abnormal opening into the vagina can be seen during a careful examination under anesthesia using special equipment. Most puppies with ectopic ureter(s) also have a bladder infection that will improve with antibiotics but the infection will return until the problem is corrected. In some cases the ureter can be surgically moved back to the normal location in the bladder and incontinence may resolve. In other cases, long standing infection of the kidney may have damaged the kidney requiring the removal of one kidney. In yet other cases the abnormality of the ureter can be corrected but the pet remains incontinent, probably due to the presence of other birth defects in the urinary system. A bladder infection can cause either a strong urge to urinate or if the bladder infection is long standing it can cause scarring of the bladder preventing it from stretching to hold urine. In this case the pet is usually not truly incontinent in that they know they are urinating, but they have such a strong urge to empty their bladder that they may urinate in abnormal locations or urinate very frequently. It is common to evaluate incontinent pets for the presence of a bladder infection. Pets with a partial blockage of the urethra with a stone or a tumor may show incontinence. If they cannot empty their bladder completely because something is blocking the path to the outside, the bladder may get so large that the back pressure of urine in the bladder actually forces some urine to leak around the blockage. In these pets the enlarged bladder can be felt on examination. Total blockage of urine flow is usually fatal in 3 to 4 days. Hormone-responsive incontinence occurs in neutered dogs of both sexes and occasionally in spayed female cats but occurs most commonly in female dogs. The pet can urinate normally, but they leak urine while resting. Physical examination and blood and urine tests are usually normal in these pets. Hormone-responsive incontinence can occur months to years after a pet is neutered. As pets age they may become incontinent. This may be due to a weakening of the muscles that hold urine in the bladder. There are many diseases that can cause a pet to create more urine than normal (polyuria) and several of these occur in older pets. If a pet has one of these diseases and often has a full bladder, the full bladder can push against the weakened sphincter and cause incontinence. Older pets can also develop senility and simply be unaware that they are dribbling urine. Dogs and cats with brain or spinal cord disease may either dribble urine or be unable to pass urine. Most often they will have other signs of nervous system disease such as muscle weakness or paralysis. Intermittent incontinence, primarily at rest, has been reported in cats of both sexes that are positive for the feline leukemia virus. How the virus causes incontinence is unknown. A less common cause of incontinence in female dogs is called vulvovaginal stenosis. It is a condition in which the vagina at the level where the urethra ends is narrowed. Occasionally when the pet urinates, some urine will get trapped in the vagina in front of this narrowed area. Then when they rise after lying down the urine pours out. This condition can be diagnosed by feeling the vagina with a gloved finger. In some dogs the narrowing can be stretched under anesthesia. The incontinence may or may not resolve as sometimes other defects are also present. Diagnosis of incontinence The tests performed to evaluate a pet with incontinence depend upon the age of the pet and on the presence or absence of other signs. It is common to collect a urine sample for bacterial culture and to see if the urine is dilute or shows evidence of an infection. Infections of the urine may be secondary to another cause of incontinence. Questions that your veterinarian will ask to help identify the cause of your pet’s problem include: Blood tests may be performed to look for evidence of kidney damage from infection or for the presence of diseases that might lead to increased urine production. Plain and/or dye X-rays or ultrasound may be performed to look at the parts of the urinary tract. Treating the incontinent patient Specific treatment of an underlying disease may resolve incontinence; for example, surgery to correct an ectopic ureter. Inappropriate urination caused by behavioral problems may be corrected with training that modifies the pet’s behavior. When no specific cause can be identified for the incontinence drugs may be given that increase the tone of the muscles that hold urine in the bladder. Some drugs that are used for this purpose include estrogen, ephedrine and phenylpropanolamine. Drug therapy for incontinence may be based on “trial” of different drugs in various doses. Since some of these drugs can have side effects so low doses are tried first. Some drugs may be slow to have an effect so as long as there are no undesirable side effects, a drug trial should continue for several weeks before the drug is considered not to be effective.
Intervertebral Disk Disease
The intervertebral disks sit between the vertebrae in the spine. They function as shock-absorbers to help dissipate the forces placed on the spine. Each disc is made up of two parts, an outer fibrous covering (the annulus fibrosus) and an inner, gelatinous portion, the nucleus pulposus.
Invertebral disc disease (IVDD) occurs when there is degeneration of the intervertebral disks. As disks degenerate, they lose some of their water content, the nucleus becomes less gelatinous and more calcified. This calcified disc is less stable and more apt to herniate (type I IVDD) or protrude (type II IVDD). Discs usually rupture or protrude in an upward direction. Sitting above the disc anatomically is the spinal cord.
Type I IVDD can occur in any area of the spinal cord. Dachshunds and other chondrodystrophic dogs (dogs with short legs and longer bodies) appear predisposed, as their disks age or degenerate more readily than most dogs. Young to middle-aged dogs are most commonly affected. Dogs less than 1 year of age rarely have intervertebral disc disease. Middle-aged to older large breed dogs can also develop disk disease (usually type II IVDD). Disc disease, in general, is rare in cats. Signs of spinal cord disease (anything from back pain, to weakness in the limbs to paralysis of the limbs) develop due to the force of the disk material hitting the spinal cord, or because of the amount of disk material that enters the spinal canal and compresses the spinal cord. The more spinal cord damage, the more severe the clinical signs. The most important determinant of prognosis in a dog with IVDD is the ability to consciously feel their limbs. If a patient can still feel his limbs, even if he can no longer move his legs, there is an 80-85% that, if surgery is performed, he will have a functional recovery and be able to walk again. IVDD is suspected as a diagnosis based on physical and neurologic exam findings, breed and history. To definitively diagnose IVDD, spinal x-rays, and either a CT scan or MRI of the spine are performed. Anesthesia is required to perform the latter two diagnostic procedures. Following advanced imaging, and the diagnosis of IVDD, surgery is then, sometimes, pursued. . General guidelines have been established for therapy depending upon severity of clinical signs. Mildly affected animals (animals back pain alone or those with mild weakness who are able to strongly walk) may be managed medically. Medical management entails strict cage confinement and appropriate pain medications for a total of 6-8 weeks. Confinement is very important to allow for healing of a degenerative disk. If, despite appropriate medical management a patient’s back pain is refractory or if the patient’s neurologic status worsens, surgery is pursued. Surgery is usually recommended in cases where animals are more severely affected (those who are unable to stand and walk). The goal of surgery is the removal of the extruded (type I IVDD) or protruded (type II IVDD).and subsequent relief of spinal cord compression. This information was made possible by funds from the Neurology Endowment at Washington State University.
Chronic Kidney Disease and Failure (CKD, CRF, CRD)
Chronic kidney disease is defined as kidney disease that has been present for months to years. Chronic renal disease (CRD), chronic renal failure (CRF), and chronic renal insufficiency refer to the same condition.
CKD is not a single disease. There are many different causes of CKD but by the time the animal shows signs of kidney disease the cause may no longer be apparent. Some potential causes of CRF include:
- congenital malformation of the kidneys (birth defects)
- chronic bacterial infection of the kidneys with or without kidney stones (pyelonephritis)
- high blood pressure (hypertension)
- diseases associated with the immune system (e.g. glomerulonephritis, systemic lupus))
- acute kidney disease, for example poisoning with antifreeze, that damages the kidneys can lead to CKD
Often the cause of CKD is unknown.
The microscopic unit of the kidney is called the nephron. Each kidney contains thousands of nephrons. When the pet is young and healthy not all nephrons are working all of the time; some nephrons are held in reserve. As the animal ages or if the kidneys are damaged, some nephrons die and other resting nephrons take over the work of those that die. Eventually all the remaining nephrons are working. When there are no extra nephrons remaining and kidney damage continues the pet will start showing signs of CKD. Because of this stepwise loss of nephrons the kidneys are able to "hide" the fact that they are damaged until the damage is severe. When 2/3 of the nephrons have been lost the pet is no longer able to conserve water and the pet passes larger amounts of dilute urine. By the time a pet has an elevation in the waste product creatinine in its blood, 75% of the nephrons in both kidneys have been lost. When blood flows through the kidneys, the kidneys act as a complex filter that removes from blood wastes that are generated from break down of food, old cells, toxins or poisons and many drugs that are given for treatment of other diseases. The wastes are removed with water as urine. Waste products than can be measured in the blood include creatinine and urea nitrogen but there are many other waste products that are not measured by blood tests. The kidneys also acts as a filter to keep "good" substances in the blood. The kidneys regulate the amount of water in the blood by excreting extra water and retaining water to prevent dehydration by varying the amount of urine that is produced. The kidneys help regulate blood pressure by saving or eliminating sodium based on how much sodium the pet is eating. The kidneys help regulate calcium and vitamin D which keep bones strong. The kidneys produce a substance that helps with the creation of new red blood cells. Because the kidneys have so many functions, when the kidneys are not working normally, there are many signs that the pet may show. By the time the pet shows signs of CKD, the damage is severe. There is no cure for CKD. The remaining nephrons are working so hard that with time they will fail as well. CKD is usually fatal in months to years but various treatments can keep the pet comfortable and with a good quality of life for months to years. Because the kidneys perform so many functions, the signs pets with CKD show can vary quite a bit. The signs may be severe or may be subtle and slowly progressive. Despite the chronic nature of the disease, sometimes signs appear suddenly. Some of the more common signs of CKD include: Signs you may see if you examine your pet include: dehydration, weight loss, pale gums and ulcers in the mouth. The signs seen in pets with CKD and the findings on examination are not specific for CKD and may be seen with many other diseases so blood and urine tests are needed to make a diagnosis of CKD. Abnormalities that are often seen on diagnostic blood and urine tests include: Sometimes bruising occurs where the blood sample was drawn as pets with CKD may have platelets that are less sticky than normal (normal platelets prevent bruising). A diagnosis of CKD can usually be made based on the signs, physical examination and blood and urine tests but other tests may be performed to look for an underlying cause for the CKD and/or to "stage" the CKD. The severity of chronic kidney disease (CKD) can be estimated based on blood waste product elevation and abnormalities in the urine such as the presence of protein. The International Renal Interest Society (IRIS) has developed a method to estimate the stages of CKD. Stages are numbered 1 through 4 where one is the least severe and four is the most severe. The higher the stage number also generally corresponds to the greater number of symptoms seen in the pet. Some treatments are recommended to be started when the pet has a certain stage of CKD. See the IRIS site for full details on staging. The severity of the pet's signs will determine what treatments are needed. Not all treatments presented below may be needed or appropriate for each pet with a diagnosis of CKD. Treatments may also be started incrementally (a few treatments are started and then based on patient response, additional treatments may be added later). The information below is not meant to be a substitute for veterinary care. Pets with severe signs may be hospitalized for fluid and intravenous drug treatment to reduce the amount of waste products in their body. Many pets with CKD will feel better in response to treatment with IV fluids but if the kidney disease is extremely severe the pet may not respond to treatment. Those pets who are still eating and not showing severe signs are treated with a variety of treatments, often introducing treatments incrementally as new signs develop. The treatment approach is often called "conservative" compared to more aggressive treatments such as hospitalization for fluid therapy, dialysis or kidney transplantation. Remember that CKD is not a disease that can be cured. Treatments are designed to reduce the work the kidneys need to perform, to replace substances that may be too low (such as potassium) and to reduce wastes that accumulate such as urea (generated by the body from proteins) and phosphorus. The initial response to conservative therapy may be relatively slow, taking weeks to months to see a response. Diet Protein restricted diets are less palatable than higher protein diets. Pets with CKD that are still eating are more likely to accept a change in diet to a protein restricted diet than are pets who are very ill and refusing most foods. Protein restricted diets are more expensive than higher protein diets. There are many pet food companies that sell kidney diets. Dr. Tony Buffington at the Ohio State University is a good source of information on available diets. http://vet.osu.edu/1442.htm select a species, a diet form and select Reduced Phosphorous/Protein for a list of diets for pets with kidney disease. Homemade diets can be fed but it is best to work with your veterinarian to formulate a diet that is balanced. It is generally agreed that feeding renal failure diets to dogs and cats with kidney disease improves their quality of live and may minimize the progression of the disease resulting in a longer life span. Studies that evaluate the effect of dietary changes on quality and quantity of life typically use commercial diets that differ in their composition of protein, phosphorus, sodium and lipids compared to maintenance diets so that positive effects are not attributable to a single component of the diet but rather to a "diet effect". A randomized, double masked, clinical study in 38 dogs with spontaneous stage 3 or 4 kidney disease, half of which were fed a kidney failure diet and the other half a maintenance diet, published in JAVMA in 2002, demonstrated improved quality and increased quantity of life in the group fed the renal failure diet. The results of a study of cats with naturally occurring stable chronic renal failure fed a diet restricted in phosphorus and protein compared to cats with CKD fed a maintenance diet reported a median survival of 633 days for 29 cats fed the renal diet compared to 264 days for 21 cats fed a regular diet. The groups were not randomly determined but based on cat & owners willingness to change to the renal diet. In a study published in JAVMA in 2006, 45 client-owned cats with spontaneous stage 2 or 3 CKD were randomly assigned to an adult maintenance diet (23 cats) or a renal diet (22 cats) and evaluated for up to 24 months. Findings included: Water Water soluble vitamins like B and C are lost in greater amounts when the pet is urinating greater amounts. Kidney diets contain increased amounts of water soluble vitamins so additional vitamins do not need to be given unless a homemade diet is being fed. Potassium Phosphorus, calcium and PTH Kidney diets typically contain reduced phosphorus and an appropriate amount of calcium but if phosphorus remains elevated when the pet is eating a kidney diet then phosphorus can be tied up in the intestinal tract so it can be eliminated in the stool. Intestinal phosphate binding agents include aluminum carbonate, aluminum hydroxide, aluminum oxide, calcium citrate, calcium acetate and calcium carbonate and sevelamer hydrochloride. Phosphate binding agents which contain calcium should not be used until blood phosphorus is normal to prevent calcium and phosphorus from combining and precipitating in tissues including the kidneys. It is not usually necessary to give additional calcium but if a pet has low blood calcium, the phosphorus should be normalized before giving calcium. Even when blood phosphorus is normalized, PTH levels are still higher than normal. The administration of low doses of vitamin D (1, 25 dihydroxycholecalciferol [calcitriol]) will suppress PTH and possibly slow the rate of progression of kidney deterioration. It is not 100% agreed that giving your pet calcitriol will slow the deterioration of the kidneys. Here are some web sites on using calcitriol http://members.bellatlantic.net/~vze2r6qt/calcitriol/ Acidosis Sodium High blood pressure (hypertension) Anemia Anemia can be treated by blood transfusion or by the administration of human erythropoietin. Erythropoietin is very effective in increasing PCV but because human erythropoietin is not exactly the same as dog and cat erythropoietin, over time, the pet may form antibodies that cause the medication to become ineffective. Canine and feline erythropoietin are currently being studied. Fats/lipids Subcutaneous Fluids Lack of Appetite Vomiting Drugs used to treat other diseases Antibiotics You are in the best position to judge what is stressful to your pet. When a pet is stressed they may drink and eat less than normal. Reduced water intake is detrimental to diseased kidneys. When possible, keep your pet calm. That might mean for example: having an in-home pet sitter if your pet is stressed by boarding, removing the pet from the household during a party or limiting contact with other animals if these situations appear to be a source of stress for your pet. Extremes in heat or cold are stresses. Certain drugs such as prednisone/cortisone make the kidneys work harder. There has been progress made in transplantation of kidneys, more for cats than for dogs. See http://www.felinecrf.com/transb.htm for a list of facilities that currently offer transplanation.Structure of the kidneys
What do the kidneys do?
CKD is progressive
Signs of CKD
Less common signs include
Diagnostic Tests
Other tests that may be performed include
What might this test show? The kidneys in pets with CRD are usually small reflecting the death of a large number of nephrons. If the kidneys are large then certain causes for the CKD should be considered such as lymphoma (cancer) of the kidneys, or an uncommon disease called amyloidosis. Some pets with signs of kidney disease who have large or normal sized kidneys may have acute kidney failure rather than CKD. The treatment and prognosis for pets with acute kidney disease differs from the treatment and prognosis of pets with CKD.
What might this test show? A biopsy is not required to make a diagnosis of CKD but the results of a biopsy may show a cause for the CKD. A biopsy is more likely to show specific information when the kidneys are big rather than small. A biopsy can be valuable in pets who develop CKD at a young age or who are of a breed known to develop congenital kidney disease. There may be specific microscopic changes in a kidney biopsy from an animal with congenital kidney disease that may suggest that related animals are also at risk for developing CKD. Knowledge that the cause of CKD is caused by congenital kidney disease does not change the treatment of the affected animal but does provide information for related animals, for example if you should remove them from a breeding program. When a biopsy is planned, usually the biopsy is collected using ultrasound or laparoscopy to see the kidney during the biopsy so that no other organs are damaged during the biopsy.
What might this test show? Bacterial infection is not a common cause of CRD but pets with CKD may develop a bacterial infection as several aspects of the pet's immune system may be less functional when the kidneys are failing. If white blood cells are observed on microscopic examination of the pet's urine, a bacterial culture of the urine should be obtained.
What might this test show? If a pet is going to under go kidney biopsy, tests may be performed in advance to evaluate the ability to stop the bleeding from the biopsy site.Treatment of CRF
Feeding of a kidney diet is usually recommended. Kidney diets contain less protein compared to other diets and the protein is high in quality. It is protein in the diet that is converted to waste products that the kidneys must remove in the urine. The higher the quality of the protein in the diet, the less wastes created for the kidneys to eliminate. Low quality protein requires the kidneys remove more wastes. which makes them work harder. Egg and meat contain higher quality protein; cereal grain protein is of lower quality which leads to more wastes for the kidneys to eliminate. Protein is used by the body to repair cells and tissues that are continually regenerating, so a pet needs some protein in their diet. By feeding a low quantity, but high quality protein diet that contains an appropriate amount of fats and carbohydrates, the pet's body can use the protein for replacing the cells and tissues and use the fat and carbohydrates for energy. Kidney diets also contain a lower amount of phosphorus. Phosphorus accumulates in the blood when the kidneys are diseased. Kidney diets control the amount of other substances that may be too high or too low in patients with CKD such as salt, potassium, magnesium and B vitamins. There are differences in the kidney diets for dogs and cats. When making diet changes it is often beneficial to gradually introduce the new diet by adding increasing amounts of the new diet while reducing the amount of the current diet over 1 to 2 weeks. The pet is more likely to accept a new diet when it is introduced gradually and it is less stressful to the kidneys to gradually adapt to changes in the diet.
body weight
PCV
urine protein-to-creatinine ratio
creatinine
potassium
calcium
parathyroid hormone concentrations.
Because pets with kidney disease cannot conserve water by making concentrated urine, their water intake is very important to prevent dehydration. Make sure they always have plenty of fresh water available. If the pet is not eating well, or is vomiting, then s(he) may not be drinking enough and may get dehydrated. Pets can be encouraged to drink by giving them flavored broths in addition to plain water. The broth should be low in sodium and its best to discuss with your veterinarian other ingredients in the broth to make sure it doesn't contain substances that will make the kidneys work harder.
Lack of appetite and increased loss of potassium in urine may result in low body potassium (hypokalemia). Cats with CKD are more likely to have low body potassium than are dogs. Cats with low potassium may develop painful muscles. Both cats and dogs may be weak when potassium is low. Cat kidney diets contain higher levels of potassium so additional supplementation is probably not needed unless the cat shows signs of muscle pain. Potassium gluconate or citrate can be given by mouth if potassium supplementation is needed. Potassium chloride is acidifying and is not recommended.
Pets with CKD usually have increased blood phosphorus. In health, phosphorus and calcium are controlled by a hormone called parathyroid hormone (PTH). PTH works with vitamin D on the intestine, kidney and bone to keep calcium and phosphorus normal. As the kidneys fail the amount of PTH in the body is elevated and the amount of vitamin D is reduced. Elevated PTH itself may be responsible for some of the signs shown by pets with CKD. PTH draws calcium and phosphorus from the bones which can weaken bones which can lead to bone fracture.
Some pets with CKD will have an acid blood pH. Kidney diets are designed to counteract the acidosis but very sick animals that are hospitalized may need addition treatment to correct the acidosis.
Diseased kidneys are less efficient at regulating sodium and sodium in turn helps control blood volume and pressure. Excess sodium can lead to water retention and not enough sodium can lead to dehydration. When changing diets that contain different amounts of sodium (kidney diets usually have less sodium than regular diets) make the change gradually over several weeks. Use caution when giving your pet table scraps or treats that may be high in sodium.
Many pets with CKD have high blood pressure. High blood pressure can contribute to further decline of kidney function and can occasionally lead to sudden blindness from retinal detachment. Ideally blood pressure should be measured by your veterinarian and hypertension confirmed before giving drugs to treat high blood pressure but measuring true blood pressure in dogs and cats can be difficult. If the pet has an elevation in blood pressure it may be due to the excitement of being examined or due to CKD. The calmer you are able to keep your pet during examination, the more reliable the readings for blood pressure. There are several drugs that may be used to manage high blood pressure including enalapril, benazepril, or amlodipine (and others). Enalapril and benazepril are in a class of drugs called <align="left"> ACE inhibitors and are sometimes used in pets with CKD that have abnormal amounts of protein in their urine even when blood pressure is normal.
The kidneys play a role in producing a hormone called erythropoietin which stimulates the production of new red blood cells. Red blood cells live about a hundred days so new cells are continually being made. Less erythropoietin is made in pets with CKD leading to anemia. The packed cell volume (PVC) (also called hematocrit) is the percentage of blood cells compared to fluid in whole blood. When the PCV is ~20 in cats and ~ 25% in dogs, anemia may contribute to lack of activity and weakness.
Certain types of fats (polyunsaturated omega 6 fatty acids) may slow the decline in kidney function are are often present in kidney diets.
Some cats and dogs with kidney disease may not drink enough to prevent becoming dehydrated and may benefit from the administration of intermittent SC fluids. If your veterinarian feels your pet may benefit from giving subcutaneous fluids, we provide some instructions on how to give SC fluids. See Cat Fluids or Dog Fluids
The accumulation of wastes in the body often decreases appetite. A goal of several of the above treatments is to reduce the amount of wastes in the blood. If the pet remains off food despite above treatments you might try different brands of renal failure diets, warming the food or adding odiferous toppings to entice the pet to eat.
Increased levels of waste products cause the pet to vomit. Your veterinarian may recommend medications that reduce nausea or act directly on brain centers to reduce the urge to vomit.
Because the kidneys are responsible for elimination of many drugs, make sure that your veterinarian is aware of any other medications you are giving your pet as these may accumulate in the body to toxic levels if the kidneys cannot eliminate them.
If the urine shows signs of infection or if a urine culture grows bacteria then antibiotics may be administered. If a urinary tract infection is involving the kidneys, the period of treatment is much longer than a infection of the bladder. Avoiding Stress
Kidney Transplantation
Determining Gender (Sex) of a Kitten
You just brought home a kitten that you intend to name Sam but your roommate tells you that you had better consider the name Samantha instead.
Determining the sex (gender) of a kitten is easy when you know what to look for.
Lift the kitten's tail. The opening just under the tail is the anus. Below the anus is the genital opening which is round in males and is a vertical slit in females. In kittens of similar size, the distance between the anus and the genital opening is greater in the male than the female.
As the male kitten grows the testicles become more apparent. The color of the kitten may suggest its gender. Almost all (but not ALL) kittens of calico (black, white and orange) or tortishell (black and orange) color are females. More orange kittens are male than female although the association between color and sex is not as strong as in the calico/tortishell colored kitten.

Laboratory: What Do Those Lab Tests Mean?
The results of laboratory tests on a patient are compared to reference ranges established by measuring the laboratory parameters in a group of normal animals. The reference ranges for each laboratory test differ between laboratories and across species. Be careful interpreting laboratory tests. An occasional animal will have a value for a laboratory test that falls outside the reference range, but the value may still be normal for that animal.
Your veterinarian will interpret laboratory tests in light of the entire evaluation of your pet. Sometimes laboratory tests need to be repeated to evaluate trends, which may provide more information than measurement of a single test.
The results of laboratory tests may be influenced by drugs your pet is receiving and some are influenced by a recent meal. Always provide your veterinarian with information about any drug your pet is receiving. Inquire when you make an appointment for veterinary care, whether you should fast your pet before the visit in case laboratory samples are collected. Complete blood count (CBC) The complete blood count also includes a measure of hemoglobin, which is the actual substance in the red blood cell that carries oxygen. There are several types of white blood cells in blood, including neutrophils (PMNs), lymphocytes, monocytes, eosinophils and basophils. Lymphocytes are produced in lymph nodes throughout the body. The other white blood cell types are produced in the bone marrow along with the red blood cells and platelets. The majority of white blood cells in circulation are neutrophils, which help the animal fight infections. Neutrophils can be decreased in pets with bone marrow disease, in some viral diseases, and in some pets receiving cancer chemotherapy drugs. Neutrophils are increased in pets with inflammation or infection of any part of the body and in pets receiving prednisone or other cortisone-type drugs. Lymphocytes also help fight infection and produce antibodies against infectious agents (viruses, bacteria, etc.). Lymphocytes may be increased in puppies and kittens with an infection, they can be decreased in pets who are severely stressed, and lymphocytes might be lost in some types of diarrhea. Certain drugs, such as prednisone (a cortisone-type drug) will decrease the number of lymphocytes in the blood stream. Monocytes may be increased in pets with chronic infections. Eosinophils and basophils are increased in pets with allergic diseases, or parasitic infections (worms, fleas, etc.). Platelets are produced in the bone marrow and are involved in the process of making a blood clot. Platelets live a few weeks and are constantly being produced by the bone marrow. Low platelet counts occur if the bone marrow is damaged and doesn’t produce them, or if the platelets are destroyed at a faster rate than normal. The two primary causes of platelet destruction are immune-mediated destruction (ITP or IMT) and DIC (disseminated intravascular coagulation). Immune-mediated thrombocytopenia happens when the animal’s immune system destroys platelets. DIC is a complex problem in which blood clots form in the body using the platelets faster than the bone marrow can produce new ones. Animals with a low platelet count bruise easily and may have blood in their urine or stool. Packed cell volume (PCV) (called hematocrit, HCT, in humans) is another measure of red blood cells. A small amount of blood is placed in a tiny glass tube and spun in a centrifuge. The blood cells pack to the bottom of the tube and the fluid floats on top. The PCV is the percent of blood, that is cells, compared to the total volume of blood. In normal dogs and cats, 40-50% of the blood is made up of blood cells and the remainder is fluid. Blood and urine tests are performed to get an initial overview of the health, and sometimes the function, of body organs. Some blood tests are very specific for a single organ, whereas other tests are affected by several organs. Blood tests are often performed as a biochemistry profile, or chemistry panel, which is a collection of blood tests to screen several organs at one time. The makeup of a biochemical profile varies with the laboratory in which it is performed. Following are some of the more commonly performed chemical tests: Albumin is a small protein produced by the liver. Albumin acts as a sponge to hold water in the blood vessels. When blood albumin is decreased, the pressure created by the heart forcing blood through the blood vessels causes fluid to leak out of the blood vessels and accumulate in body cavities such as the abdominal cavity or in tissues as edema. Albumin is decreased if the liver is damaged and cannot produce an adequate amount of albumin or if albumin is lost through damaged intestine or in the urine due to kidney disease. The only cause of increased albumin is dehydration. Alkaline phosphatase originates from many tissues in the body. When alkaline phosphatase is increased in the bloodstream of a dog the most common causes are liver disease, bone disease or increased blood cortisol either because prednisone or similar drug is being given to the pet or because the animal has Cushing's disease (hyperadrenocorticism). In cats, the most common causes of increased alkaline phosphatase are liver and bone disease. ALT is an enzyme produced by liver cells. Liver damage causes ALT to increase in the bloodstream. ALT elevation does not provide information as to whether the liver disease is reversible or not. Amylase is an enzyme produced by the pancreas and the intestinal tract. Amylase helps the body breakdown sugars. Amylase may be increased in the blood in animals with inflammation (pancreatitis) or cancer of the pancreas. Sometimes pancreatitis is difficult to diagnose and some dogs and cats with pancreatitis will have normal amounts of amylase in the blood. Lipase is another pancreatic enzyme which is responsible for the breakdown of fats and which may be increased in patients with pancreatic inflammation or cancer. Bile acids are produced by the liver and are involved in fat breakdown. A bile acid test is used to evaluate the function of the liver and the blood flow to the liver. Patients with abnormal blood flow to the liver, a condition known as portosystemic shunt will have abnormal levels of bile acids. The bile acid test measures a fasting blood sample and a blood sample two hours after eating. Bilirubin is produced by the liver from old red blood cells. Bilirubin is further broken down and eliminated in both the urine and stool. Bilirubin is increased in the blood in patients with some types of liver disease, gallbladder disease or in patients who are destroying the red blood cells at a faster than normal rate (hemolysis). Large amounts of bilirubin in the bloodstream will give a yellow color to non-furred parts of the body, which is called icterus or jaundice. Icterus is most easily recognized in the tissues around the eye, inside the ears and on the gums. BUN (blood urea nitrogen) is influenced by the liver, kidneys, and by dehydration. Blood urea nitrogen is a waste product produced by the liver from proteins from the diet, and is eliminated from the body by the kidneys. A low BUN can be seen with liver disease and an increased BUN is seen in pets with kidney disease. The kidneys must be damaged to the point that 75% of the kidneys are nonfunctional before BUN will increase. Pets that are severely dehydrated will have an increased BUN as the kidneys of a dehydrated patient don’t get a normal amount of blood presented to them, so the waste products do not get to the kidneys to be eliminated. Calcium in the bloodstream originates from the bones. The body has hormones, which cause bone to release calcium into the blood and to remove calcium from the blood and place it back into bone. Abnormally high calcium in the blood occurs much more commonly than low calcium. High blood calcium is most commonly associated with cancer. Less common causes of elevated calcium are chronic kidney failure, primary hyperparathyroidism which is over-function of the parathyroid gland, poisoning with certain types of rodent bait and bone disease. Low blood calcium may occur in dogs and cats just before giving birth or while they are nursing their young. This is called eclampsia and occurs more commonly in small breed dogs. Eclampsia causes the animal to have rigid muscles which is called tetany. Another cause of low blood calcium is malfunction of the parathyroid glands which produce a hormone (PTH) that controls blood calcium levels. Animals poisoned with antifreeze may have a very low blood calcium. Cholesterol is a form of fat. Cholesterol can be increased in the bloodstream for many reasons in dogs. It is much less common for cats to have increased cholesterol. Some of the diseases that cause elevated cholesterol are hypothyroidism, Cushing's disease, diabetes and kidney diseases that cause protein to be lost in the urine. High cholesterol does not predispose dogs and cats to heart and blood vessel disease as it does in people. Creatinine is a waste product that originates from muscles and is eliminated from the body by the kidneys. An elevation of creatinine is due to kidney disease or dehydration. Both creatinine and BUN increase in the bloodstream at the same time in patients with kidney disease. Creatinine kinase (CK) is released into the blood from damaged muscle. Elevation of creatinine kinase therefore suggests damage to muscle including heart muscle. Glucose is blood sugar. Glucose is increased in dogs and cats with diabetes mellitus. It may be mildly increased in dogs with Cushing's disease. Glucose can temporarily increase in the blood if the dog or cat is excited by having a blood sample drawn. This is especially true of cats. A quick test to determine whether a glucose elevation is transient or permanent is to look at the urine. If the glucose is chronically elevated there will be an increased amount of glucose in the urine as well. Low blood sugar occurs less commonly and can be a sign of pancreatic cancer or overwhelming infection (sepsis). Low blood sugar can cause depression or seizures. Low blood sugar can be seen if the blood sample is improperly handled. Red blood cells will use glucose so typically red blood cells are removed from the blood sample and the clear part of the blood (plasma or serum), is used for analysis. Phosphorus in the bloodstream originates from bones and is controlled by the same hormone, PTH (parathyroid hormone) which controls blood calcium. Phosphorus is increased in the bloodstream in patients with chronic kidney disease. Like BUN and creatinine, phosphorus increases in these patients when about 75 percent of both kidneys is damaged. Potassium is increased in the bloodstream in the pet with acute kidney failure such as kidney failure caused by antifreeze poisoning, in dogs with Addison's disease and in animals with a ruptured or obstructed bladder. Potassium is lost from the body in vomit, diarrhea and urine. Pets that are not eating may have a low blood potassium. Low blood potassium can cause the pet to feel weak. Cats with low potassium may develop painful muscles. Sodium may be slightly increased in the blood if the patient is dehydrated although many dehydrated dogs and cats have a normal blood sodium. Low blood sodium is most commonly seen with Addison's disease (hypoadrenocorticism). Total protein includes albumin and larger proteins called globulins. Included in the globulins are antibodies which are protein molecules. Total protein can be increased if the dog or cat is dehydrated or if the pet's immune system is being stimulated to produce large amounts of antibody. Total protein is decreased in the same situations which reduce albumin or if the pet has an abnormal immune system and cannot produce antibodies. Urinalysis: A urine sample can provide information about several organ systems. The concentration, color, clarity and microscopic examination of the urine sample can provide diagnostic information. Urine may be obtained by catching a sample during normal urination, by passing a catheter into the bladder or by placing a small needle through the body wall into the bladder, a procedure called cystocentesis. Depending upon why the urine sample is being collected, one collection method may be preferred over another. Inquire at the time you make an appointment for veterinary care if a urine sample may be collected. Preventing your pet from urinating prior to the appointment will assure that your pet’s bladder will contain urine for sampling.
The complete blood count measures the number of cells of different types circulating in the bloodstream. There are three major types of blood cells in circulation; red blood cells (RBC), white blood cells (WBC), and platelets. Red blood cells are produced in the bone marrow, which is the soft center of bones. RBCs pick up oxygen brought into the body by the lungs, and bring that oxygen to cells throughout the body. Red blood cells live in the blood stream for about 100 days although the actual time varies with the type of animal. Old red blood cells are removed from the blood stream by the spleen and liver. Red blood cell numbers can be decreased (anemia) if they are not produced in adequate numbers by the bone marrow, if their life span is shortened (a condition called hemolysis), or if they are lost due to bleeding. Increased red blood cell numbers is called polycythemia and is usually due to concentration of the blood due to dehydration.
Lyme Disease
What is Lyme disease?
Lyme disease is caused by the corkscrew-shaped bacteria, Borrelia burgdorferi which is also called a spirochete. The bacteria are carried by ticks which transmit the infection when they feed on animals and humans. The disease can cause generalized illness in animals and humans worldwide.

| In the United States, Lyme disease occurs predominantly on the Pacific coast and in the Midwest, and Atlantic coast states. Regions in which the disease occurs commonly are called endemic regions. About 75% of dogs living in endemic regions are exposed to infected ticks, but only a small percentage of exposed dogs develop signs of disease. |
Lyme disease was first described in 1975 when an unusual outbreak of rheumatoid arthritis occurring in children was reported in Lyme, Connecticut. In 1982, the bacteria Borrelia burgdorferi was determined to be the cause of that outbreak. Since Lyme disease was first described in the early 1980's, the frequency of occurrence of disease has increased twenty-five fold. Today, Lyme disease is the most common vector-borne (transmitted by insects or arthropods) disease occurring in people and probably in dogs in the United States. Dogs are most frequently infected with the Lyme disease bacteria, but infections can also occur in horses, cattle, and cats. How is Lyme disease transmitted? If your pet is diagnosed with Lyme disease you are not at risk of getting Lyme disease directly from your pet. The bacteria increase to high levels in the blood of wildlife whereas humans and domestic animals develop very low levels of the bacteria in their blood and these low levels will not infect a feeding tick. Researchers have learned that infected ticks must feed for about 24 hours to transmit the bacteria to a susceptible animal so quick removal of ticks from your pet reduces the chance of infection. Clinical signs Diagnosis Treatment Prevention There is a vaccine approved for use in dogs for Lyme disease prevention. Most authors of veterinary articles on Lyme disease do not recommend vaccinating dogs in non-endemic areas. Not all authors agree on how effective the vaccine is in preventing Lyme disease and not all authors agree that the vaccine should be given in endemic regions. The vaccine can cause some blood tests for Lyme disease to become positive. For more information about tick control products or Lyme disease, consult your veterinarian. References: This topic was written by Wendy Harless, Oregon State University, class of 2002 with the guidance of Dr.Diana Stone, Washington State University.
The bacteria live in mice, deer and other small mammals. The type of ticks that can transmit the bacteria from these wildlife to humans and domestic animals are the Ixodes ticks. The bacteria replicate (increase in number) in the wildlife without causing them to become sick. When a tick feeds on the infected wildlife the tick picks up the bacteria, then they transmit the bacteria to another animal the next time they feed.
The most common sign of Lyme disease in dogs is arthritis, which causes sudden lameness, pain ands sometimes swelling in one or more joints. Other signs that may be seen include fever, lack of appetite, dehydration, inactivity, and swollen lymph nodes. In severe cases, the infection can cause kidney failure and death although this does not occur commonly in dogs. The signs of heart and nervous system dysfunction seen in infected humans are not often seen in animals.
A diagnosis of Lyme disease is usually made based upon a history of being in an endemic area, signs of arthritis and favorable response to treatment. There is a blood test that measures antibodies to the bacteria but many dogs that live in endemic regions will have a positive blood test. A positive blood test just means that the dog was exposed to Borrelia burgdorferi but not all dogs that are exposed will show signs of disease. Early in the disease dogs may not yet have a positive blood test. Dogs that have been vaccinated for Lyme disease may have a positive blood test depending upon the type of blood test that is performed. There are several other causes of arthritis that occur in dogs that must also be considered.
Borrelia burgdorferi is easily treated with antibiotics. The signs of Lyme disease usually regress rapidly in response to treatment. If the disease remains untreated the disease becomes chronic and can cause kidney damage although dogs are much less likely to develop chronic disease than are people.
Animals in endemic areas are at greatest risk for infection. The best method of prevention is to avoid tick infested areas, especially in the spring when the young ticks are most active. When returning from a tick-infested area do a thorough search for ticks on both yourself and your animals. Ticks should be removed carefully with a tweezers, pinching the tick near the point they enter the skin. There are also many highly effective veterinary products that will kill ticks on your dog before the tick can transmit the bacteria. Remember that early removal of ticks reduces the chance that the tick will transmit Lyme disease.
For additional information on Lyme disease see: the Centers for Disease Control (CDC) website
Canine Lymphosarcoma (Lymphoma, LSA)
Incidence/cause
LSA, a tumor caused by a cancerous proliferation of lymphocytes (cells that normally function in the immune system), is one of the most common tumors seen in dogs. It affects dogs of any breed and age, although most dogs will be middle-aged or older at the time of diagnosis; Golden retrievers are considered a breed at increased risk of developing LSA. The cause of LSA in dogs, as is true for most canine tumors, is not known.
The presentation of dogs with LSA is highly variable as lymphocytes can be found in virtually any organ in the body. Nonetheless, the most common form (referred to as stages) of LSA causes a non-painful enlargement of one or more lymph nodes that can be seen or felt from the body surface. Occasionally, a lymph node becomes large enough to impair function (obstruction of blood flow or airway, for example). Other forms of LSA can involve the liver, spleen, bone marrow and gastrointestinal tract, skin or nervous system (and other organs) and the clinical signs will reflect the organ system involved (e.g. vomiting or diarrhea with gastrointestinal forms; weakness or pale mucous membranes and others that reflect impaired production of blood cells from the bone marrow); many dogs will simply feel ill (lose appetite, become lethargic) with any of the different forms. In some dogs, lymph node enlargement is an incidental finding when an otherwise healthy-appearing dog is seen by a veterinarian for an unrelated reason (e.g. vaccination). Stage I: single lymph node enlarged LSA is viewed as a systemic disease, and as such is not really viewed to "spread" to other organs. This tumor is not generally viewed as a curable tumor in dogs, although occasional dogs will experience what seems to be a cure with appropriate treatment (see below). A dog can start with one stage of the disease and progress over time to another (usually more advanced) stage of LSA. Because of the organs that LSA commonly involves, staging a dog with a LSA can involve aspiration of one or more lymph nodes, thoracic radiographs abdominal radiographs or ultrasound (to look for big nodes in the abdomen and to look at the liver and spleen), or bone marrow examination. Often, obtaining blood for a complete blood count and biochemical profile, and a urinalysis will be advised as these can help assess overall health and provide information that potentially influences treatment recommendations. Sometimes, special stains to determine if the LSA is of B-cell or T-cell origin (B-cells and T-cells are specific types of lymphocytes) are recommended because of prognostic significance, although treatment recommendations are the same for either type. The mainstay of treatment of LSA is administration of chemotherapy drugs; the best responses in terms of length of tumor control and survival are generally seen with protocols that entail administration of more than one chemotherapy drug, although there are approaches that involve administration of a single drug. Chemotherapy drugs commonly used include: doxorubicin, vincristine, cyclophosphamide, prednisone, and L-Aspariginase, but many others are also used. In some dogs with very localized disease, surgery or radiation therapy can play a role in treatment, although chemotherapy is still often recommended in these cases. The prognosis of dogs with LSA is highly variable, and depends on the clinical stage (ill dogs fare more poorly than dogs that feel well, and dogs with Stage V disease are generally considered to have a poorer prognosis), the type of tumor (dogs with B-cell LSA usually do better than dogs with T-cell LSA). Most dogs treated with chemotherapy will experience a remission, a period in which there is no detectable cancer and the dog feels well. Remission times are variable, but most dogs with the lymph node forms of LSA will have initial remissions lasting in the range of 6-9 months before evidence of the tumor is seen again; second remissions can be achieved in many of these dogs, but any subsequent remission is expected to be shorter in duration than the first remission. Survival times for most dogs treated with combination chemotherapy protocols are in the range of approximately 1 year. And even though an individual dog will have received a lot of chemotherapy over that year, their quality of lfe is generally very good. Statistics, while useful, can never predict how an individual dog will fare with or without specific treatment. New protocols are tried with great regularity in canine lymphoma but results have been similar with each drug regime investigated. Most likely our survivals will always be similar until we either accept greater toxicity (meaning most dogs will be very sick from the treatment and some may even die), or a completely novel treatment is invented. Using half or whole body radiation therapy may prove helpful. The development an antibody specific for dog lymphoma, which could recognize all dog lymphomas and yet no normal lymphocytes, and be attached to a toxin or other cell killing mechanism, is a far off dream. LSA is one of the most chemotherapy-responsive tumors seen in veterinary medicine, and most dogs tolerate chemotherapy very well with minimal impact on their quality of life. If you notice fast growing lumps on your dog that seem to be in the area of the major joints (at the neck, in front of the shoulders, in the armpits, at the back of the knees or in the groin) have your dog examined soon by a veterinarian even if he feels well. Remember, lower stage disease, and dogs that feel well, will do better with treatment than dogs that are ill and/or have more advanced disease.What you might see/ Clinical presentation
Lymph node staging
Stage II: multiple nodes enlarged on either the front half or back half of the body
Stage III: multiple nodes enlarged on both front and back halves of body
Stage IV: involvement of the liver and/or spleen
Stage V: bone marrow involvement, or involvement of other organs (e.g. gastrointestinal, skin, nervous system)
Each numbered stage can be further divided into substages, of which there are two: a and b. Patients with substage a feel well while patients with substage b are ill.Biological behavior of LSA
Clinical staging (determination of the extent of the tumor)
Treatment options
Prognosis
Future treatment options:
Key points
Feline Lymphosarcoma (Lymphoma, LSA)
Incidence/Cause
Lymphosarcoma is a tumor caused by a cancerous proliferation of lymphocytes or, cells that normally function in the immune system. This is a very common tumor in cats and can present in a variety of ways. At one time, feline leukemia virus (FeLV) was a leading cause of LSA in cats and typically young cats were infected. Now that the incidence of FeLV has decreased cats still develop LSA but it is generally older cats and different forms. The Feline aids virus (FIV) has also been shown to increase the risk of a cat developing LSA six times over a non-infected cat. Any breed of cat can develop LSA. The cause of the disease unrelated to FeLV or FIV is unknown although environmental smoke exposure has been found to increase a cat’s risk of LSA, and a possible link to long standing inflammatory disease has long been theorized.
Cats with LSA present with a variety of signs because lymphocytes can be found in nearly every organ in the body. Also, cats seem to have more forms of LSA in atypical locations or not in normal lymphoid tissues, as compared to other species. Most species including man present with large lymph nodes, but this is a rare form of LSA in cats. Young cats typically present for masses in the chest cavity and owners notice signs of difficulties breathing or vomiting of food. Older cats develop the tumor in their intestines quite commonly and owners may notice signs such as weight loss, diarrhea or vomiting. They also can however develop LSA in areas as diverse as the nasal passages, kidneys, spinal cord, liver, eyes, or a single lymph node, and the signs seen will be more specific for the organ affected. Because cats present with such a variety of organs affected there is no valid staging system for feline LSA and a cat diagnosed with the disease will more likely be staged by the organ affected (eg. gastrointestinal LSA, mediastinal LSA etc.) Even though many cats present with only a single site of involvement, LSA is viewed as a systemic disease. Lymphocytes in their normal functioning capacity travel throughout the body and as a cancer the disease is also moving though not in a classical sense "metastasizing". Even if a tumor diagnosed as LSA has been surgically removed the disease is not gone. Because of the organs that LSA commonly involves, staging a cat with a LSA can involve aspiration of one or more lymph nodes or masses, thoracic radiographs abdominal radiographs or ultrasound (to look for big nodes in the abdomen and to look at the liver and spleen), or bone marrow examination. Obtaining blood for a complete blood count and biochemical profile, FeLV, FIV, and a urinalysis is always advised as these can help assess overall health and provide information that potentially influences treatment recommendations. Sometimes, special stains to determine if the LSA is of B-cell or T-cell origin (B-cells and T-cells are specific types of lymphocytes) are recommended because of prognostic significance, although treatment recommendations may be the same for either type. Staging the disease can be critical in choosing treatment protocols. Chemotherapy should always be considered a critical part of the treatment for LSA. The best responses in terms of length of tumor control and survival are generally seen with protocols that entail administration of more than one chemotherapy drug, although there are approaches that involve administration of a single drug. Chemotherapy drugs commonly used include: doxorubicin, vincristine, cyclophosphamide, prednisone, and L-Aspariginase, but many others are also used. Some protocols are very aggressive and relatively short (six month total) and others are less aggressive but extend for one to two years. The decision of which protocol is to be used does depend on the results of the tumor biopsy (not all LSA is the same) and the staging results. Thankfully, the chemotherapy generally act quickly so that even cats with sever signs can have relief fairly soon after starting therapy (sometimes as quickly as 24 hours). Surgery is sometimes recommended as a part of the treatment but this is usually either to reach a diagnosis or to remove a potentially life threatening problem (for example intestinal rupture due to a tumor mass). Surgery is never curative and should always be followed by chemotherapy to best extend the cat’s life. Radiation can also play a role in the treatment of very localized LSA. The primary site most benefiting from radiation therapy is nasal LSA. Cats with LSA have unpredictable responses and survivals. Depending on the site of the tumor, mean survivals with chemotherapy range from 6-9 months. The problem is that this is only an average and most cats tend to do either much worse or much better. Young cats, FeLV negative, with mediastinal LSA are quite regularly cured with chemotherapy; cats with LSA in their central nervous system typically have a bad prognosis, but most other forms of LSA in cats have unpredictable outcomes. Generally it is best to at least try a chemotherapy protocol because it may be the only way to see how an individual cat will do. Cats often do not enjoy receiving chemotherapy, but veterinary oncologist try hard to make the regime tolerable for each feline patient even if it means modifications in a protocol. New protocols are tried in feline lymphoma but results have been similar with each drug regime investigated. Most likely our survivals will always be similar until we either accept greater toxicity (meaning most cats will be very sick from the treatment and some may even die), or a completely novel treatment is invented. Using half or whole body radiation therapy may prove helpful. The development an antibody specific for cat lymphoma, which could recognize all cat lymphomas and yet no normal lymphocytes, and be attached to a toxin or other cell killing mechanism, is a far off dream. LSA is one of the most chemotherapy-responsive tumors seen in veterinary medicine and cats can tolerate chemotherapy relatively well, or protocols can be modified so that an individual cat can maintain a good quality of life while on chemotherapy. Unfortunately we have few strong predictors of which cats will have good responses to chemotherapy and long survivals, and survival is therefore difficult to estimate at the outset. Often the only way to know how a cat will respond to treatment, is to start treatment. What you might see/ Clinical presentation
Biological behavior of LSA
Clinical staging (determination of the extent of the tumor)
Treatment options
Prognosis
Future treatment options
Key points
Canine Mast Cell Tumors
Incidence/Cause
Mast cell tumors (MCT) in dogs are very common, accounting for approximately 20% of all skin tumors in dogs. For most dogs, the underlying cause promoting the development of the tumor is not known. Mast cell tumors can arise from any skin site on the body, and can have a variety of appearances. Veterinary oncologists recommend that before any skin lump is removed, the cells from the mass be collected for examination to rule out the lump as a mast cell (or other malignant) tumor. And mast cells are something that are easily identified on aspiration.
MCT most commonly are seen as solitary lumps or masses in or underneath the skin; occasional dogs can have multiple masses from MCT. MCT can look like just about anything, ranging from benign-appearing lumps (such as a lipoma), to more angry or ulcerated lumps, masses with a stalk or focal thickenings in the skin. MCT may change quickly in size (become larger then smaller ) because of reactions around the mass. Some dogs may have signs of systemic disease, which can be caused by some of the biologically active compounds found within mast cells. In most cases, evidence of a MCT is easily generated by examination of a fine-needle aspirate of the suspect mass, and aspiration is advised before removal of a mass to be sure it is not a MCT (or other skin malignancy), a finding that would demand a more aggressive surgical removal. Often, obtaining blood for a complete blood count and biochemical profile, and a urinalysis will be advised as these can help assess overall health and provide information that potentially influences treatment recommendations. Most mast cell tumors are considered locally invasive, and can be difficult to remove completely because of the extent of local spread. The behavior of mast cell tumors reflects their grade (a term used by pathologists and oncologists to describe such things as how-well differentiated a tumor is, how frequently it is dividing, how invasive to adjacent structures, and other criteria). Mast cell tumors have 3 grades, with grade I being the least aggressive and least likely to spread to other organs (metastasize), and grade III being highly aggressive tumors with a high likelihood of metastasis; most grade II tumors tend not to metastasize, although they can do so. Mast cell tumors show a predilection to spread to regional lymph nodes, liver, spleen, and bone marrow. Because of the organs to which these tumors like to spread (metastasize) to, staging a dog with a mast cell tumor (usually reserved for occasional grade I tumors, most grade II tumors and all grade III tumors) entails collection of cells from regional lymph nodes for microscopic examination, imaging the thorax (radiographs) and abdomen (radiographs, abdominal ultrasound) for enlargement of lymph nodes, liver or spleen, and some assessment of bone marrow involvement, either a bone marrow collection for microscopic examination, or examination of the white blood cells for circulating mast cells (interpreted to mean that mast cells are in the bone marrow). Surgical removal is the mainstay of treatment of canine mast cell tumors. Because of their locally invasive behavior, wide margins of what appears to be normal tissue around the tumor needs to be removed to increase the likelihood that the tumor has been completely removed. For mast cell tumors that were not, or because of location, could not be completely removed, radiation therapy is often the best treatment for residual disease, although a more aggressive second surgery is possible for some dogs. Chemotherapy is sometimes used to treat mast cell tumors, but chemotherapy is usually reserved for dogs with grade III tumors; mast cell tumors are notoriously unpredictable tumors with regards to response to chemotherapy. In addition to treatment of the tumors, some dogs will be treated with medications that tend to help fight the secondary effects of the tumor. These usually include drugs like prednisone, an anti-histamine like Benadryl, and an antacid type medication like Pepcid. The prognosis for completely removed grade I and grade II tumors is excellent. The prognosis for incompletely removed grade I and II tumors treated with radiation therapy after surgery is also excellent with approximately 90-95% of dogs having no recurrence of tumor within 3 years of receiving radiation therapy. The prognosis for dogs with grade III tumors is considered guarded as local recurrence and/or spread is likely in most dogs. If your dog is diagnosed with a grade III Mast cell tumor most likely chemotherapy will be recommended as at least part of the protocol. Drugs used at WSU include Lomustine and Vinblastine. Mast cell tumors have been examined for mutations in a certain gene known as c-kit. This c-kit gene belongs to a family of genes codes for receptor tyrosine kinases. Receptor tyrosine kinase inhibitors are an active part of cancer treatment research in the human field and these drugs are being looked at treatments for canine Mast cell tumors as well. No drug is currently available commercially. Dogs that develop Mast cell tumors seem to like to develop more of them and this is not necessarily the same as metastasis. So any dog diagnosed with a mast cell tumor must be watch closely in the future for the development of new tumors. As long as tumors are caught when small, surgical removal is usually adequate for treatment. Mast cell tumors can also be very unpredictable tumors. Even grade I and II tumors can behave aggressively in terms of metastasizing and or being difficult to control locally, in any given individual dog. Statistics, while useful, can never predict how an individual dog will fare with or without specific treatment.What you might see/ Clinical presentation
Biological behavior of mast cell tumors
Clinical staging (determination of the extent of the tumor)
Treatment options
Prognosis
Future treatment options
Key points
Giving Oral Medications to Your Cat
This information is not meant to be a substitute for veterinary care. Always follow the instructions provided by your veterinarian.
Your veterinarian will tell you if your cat's medication(s) can be given with food or if it must be given on an empty stomach. If the tablet or capsule can be given with food, you may make a "meatball" by placing the medication in the center of a small ball of canned cat food or cheese. Always give a test "meatball" to your cat to make sure she is willing eat it and also to see if she chews it or gulps it whole. Cats are more likely to chew their food than are dogs, so cats often will eat the "meatball" and spit out the tablet or capsule. This causes the tablet or capsule to partially dissolve and become very hard to handle. If the cat bites into the tablet or capsule, which will leave a bad taste in her mouth, she will be harder to medicate on the second attempt. So, you will have to decide what works best with your cat.
The following instructions are presented to help you give medications if you cannot give the medicine in a "meatball". Use caution when giving a cat oral medication to avoid a bite. A cat's mouth contains many bacteria and cat bites are often deep punctures. If you are bitten by your cat, clean the wound thoroughly and seek medical attention. Medications for oral administration may be in pill, capsule or liquid form. Hold the cat's head from the top using your left hand if you are right-handed. The cat's cheek-bones (called zygomatic arches) provide a convenient handle by which to hold the head firmly without causing the cat any discomfort. Tilt the head back and the cat will often drop its lower jaw open. Hold the pill or capsule in your right hand between your thumb and index finger. You can place one of the remaining fingers on your right hand on the lower incisors to keep the lower jaw open. Keep your finger over the small incisor teeth NOT over the sharp fangs (canine teeth). Drop the pill or capsule as far back over the tongue as possible, then immediately close the mouth and blow on the cat's nose which will encourage them to swallow. If the cat does not open its mouth when you tilt back the head, holding the pill as before between the thumb and index finger... ...use the middle finger of the same hand holding the pill or capsule, to pry open the lower jaw. Place your middle finger over the small incisor teeth NOT over the sharp fangs (canine teeth)... ...and pull open the lower jaw. Keep the middle finger in place to hold the lower jaw open (3), then either drop the pill or capsule as far back on the tongue as possible, or the index finger (1) and thumb (2) can be used to push the pill over the back of the tongue. IMPORTANT: If you use your thumb and index finger to push the pill over the base of the tongue, your fingers will be inside the cat's mouth and you must work rapidly to avoid getting bit. Close the mouth and stroke the cat's neck or blow sharply on his/her nose to encourage the cat to swallow There are several styles of pilling devices that can be used to place a pill or capsule over the base of the tongue so that you do not have to place your fingers in the cat's mouth. There are several ways to hold the pilling device. You can hold the device between your thumb and middle finger, with the index finger positioned to "push" the trigger. Or to prevent premature release of the pill, move the index finger to push the trigger just before dislodging the pill in the back of the throat. You could also hold the device between curled fingers and palm either with the thumb positioned to "push" the trigger. Or to prevent premature release of the pill, you may move the thumb to push the trigger just before dislodging the pill in the back of the throat. Or you can hold the device between the index and middle fingers with the thumb positioned to "push" the trigger. Tilt the head back and the cat will often drop their lower jaw open. Insert the pill at the end of the pilling device over the base of the tongue. If the cat doesn't open it's mouth, use the middle finger of the hand holding the pilling device to open the lower jaw. Insert the pill at the end of the pilling device over the base of the tongue. Push the plunger on the pilling device with your thumb or index finger to deposit the pill far back in the cat's mouth. Liquid medications are given in a pouch between the teeth and cheek. The medication is quickly squirted into this pouch, the mouth is held closed and the neck stroked or the nose sharply blown on to encourage the cat to swallow. Liquids are more likely to accidentally enter the windpipe compared to pills or capsules. To avoid the cat inhaling liquid into the windpipe, DO NOT tilt the cat's head backward. If you find it difficult to give your cat a pill or capsule, speak to your veterinarian about suspending the pill or capsule into a liquid. Some medications can be suspended in liquid while others lose their effectiveness when placed in a suspension. Always talk to your veterinarian before altering the medication.



















Giving Oral Medications to Your Dog
This information is not meant to be a substitute for veterinary care. Always follow the instructions provided by your veterinarian.
In the photographs below, the dog's nose is pointed to your right.
Variations on these instructions exist.
Your veterinarian will tell you if your dog's medication(s) can be given with food or if it must be given on an empty stomach. If the tablet or capsule can be given with food, you may make a "meatball" by placing the medication in the center of a small ball of canned dog food or cheese. Always give a test "meatball" to your dog to make sure she is willing eat it and also to see if she chews it or gulps it whole. Dogs are more likely to gulp the "meatball" without chewing. If they do chew the "meatball" and spit out the pill, the tablet or capsule will partially dissolve and become very hard to handle. If the dog bites into the tablet or capsule, which will leave a bad taste in her mouth, she will be harder to medicate on the second attempt. So, you will have to decide what works best with your dog.
The following instructions are presented to help you give medications if you cannot give the medicine in a "meatball". Use caution when giving a dog oral medication to avoid a bite. A dog's mouth contains many bacteria. If you are bitten by your dog, clean the wound thoroughly and seek medical attention. Medications for oral administration may be in pill, capsule or liquid form. Hold the dog's head from the top using your left hand if you are right-handed. If the dog has a long nose hold the upper jaw between thumb and index finger. If the dog has a short nose, hold the head like a cat (see giving oral medications to a cat). Tilt the head back. Dogs have stronger jaw muscles than cats and unlike the cat, the lower jaw does not usually drop open far enough to place the pill or capsule over the base of the tongue. Gently fold the upper lip over the teeth as you open the mouth. If the dog bites down with your hand in her mouth, she will bite her lip and will not bite your hand. Place your thumb on the roof of the dog's mouth. You do not have to fold the dog's lip over their teeth but this does reduce the chance of you being bit. Hold the pill or capsule in your right hand between your thumb and index finger. Use the middle finger of your right hand to pull open the lower jaw. Keep your middle finger over the small incisor teeth NOT over the sharp fangs (canine teeth). Drop the pill or capsule as far back over the tongue as possible, then immediately close the mouth and blow on the dog's nose which will encourage her to swallow. If you are unable to get the pill far enough over the base of the tongue, the dog will spit it out. You may need to use your index finger and thumb to push the pill over the back of the tongue. IMPORTANT: If you use your thumb and index finger to push the pill over the base of the tongue, your fingers will be inside the dog's mouth and you must work rapidly to avoid getting bit. Close the mouth and stroke the dog's neck or blow sharply on his/her nose to encourage the dog to swallow. Notice the dog's lip is still folded over the upper teeth to protect the hand from being bitten. There are several styles of pilling devices that can used to place a pill or capsule over the base of the tongue so that you do not have to place your fingers in the dog's mouth. See section on pilling a cat for details. Liquid medications are given in a pouch between the teeth and cheek. The medication is quickly squirted into this pouch, the mouth is held closed and the neck stroked or the nose sharply blown on to encourage the dog to swallow. Liquids are more likely to accidentally enter the windpipe compared to pills or capsules. To avoid the dog inhaling liquid into the windpipe, DO NOT tilt the dog's head backward. If you find it difficult to give your dog a pill or capsule, speak to your veterinarian about suspending the pill or capsule in a liquid. Some medications can be suspended in liquid while others lose their effectiveness when placed in a suspension. Always talk to your veterinarian before altering the medication.








Canine Osteosarcoma (OSA)
Incidence/Cause
OSA is the most common primary bone tumor of dogs and is estimated to account for roughly 85% of tumors in the canine skeleton. It is most often a tumor of the front limb with tumors near the "wrist" (in the radius or ulna) common and tumor in other sites of the front and rear leg somewhat less common. Another rule of thumb often stated is that these tumor occur away from the elbow and towards the knee. OSA can, however, occur in any bone. Middle aged to older large to giant breed dogs are most often affected by the form of tumor involving the long bones such as the radius, ulna, humerus, femur and tibia. The cause of this tumor is largely unknown.
The most common sign seen in dogs with OSA is lameness. Lameness may develop suddenly (for example, after vigorous activity), or may develop more slowly. Depending on the location of the tumor, a swelling or mass-like effect could be seen in the affected leg. Any lameness in a large-breed dog that does not promptly resolve with symptomatic therapy should be further investigated (examination, radiographs). OSA is both a locally invasive tumor and a tumor with a high likelihood of spread (metastasis) to other organs, most commonly the lung, although metastasis to other organs is possible. Most (approximately 90-95%) of dogs with OSA are considered to have metastasis at the time of their diagnosis, although metastasis will only be evident at the time of diagnosis in approximately 10% of dogs and in others the metastatic tumors are considered to be microscopic. Tumors in bone are quite painful to affected dogs, accounting for the lameness that is seen as the most common presenting complaint in affected dogs. Radiographs of the affected leg, and radiographs of the thorax are the most critical elements of clinical staging; dogs with enlarged lymph nodes will also typically have the lymph nodes sampled for microscopic examination. Radiographs of affected legs are often highly suggestive of the diagnosis, and biopsies are not necessary for all dogs with compatible lesions on radiographs. Often, obtaining blood for a complete blood count and biochemical profile, and a urinalysis will be advised as these can help assess overall health and provide information that potentially influences treatment recommendations. When aggressive therapy is being considered, a CT examination of the lungs will also be recommended to screen the lungs for metastasis even more precisely than the radiographs can show us. Amputation to remove the primary tumor, combined with chemotherapy to treat the metastatic disease we can’t yet see, is the best treatment for preservation of quality (relief of pain) and quantity of life for dogs with the limb form of OSA. Not every dog is a candidate for amputation and the decision to amputate is often difficult for owners. Dogs with severe arthritis in the unaffected limbs, or weakness due to neurologic disease may not be candidates for amputation but most other dogs are. Dogs can function on three legs much better than most owners think. Some institutions offer limb-sparing surgery, in conjunction with chemotherapy, but this can only be done when the tumor is in the radius or ulna near the carpal joint (wrist). Not every owner is prepared for the expense and time commitment to chemotherapy either. Generally therapy is done once every 3-4 weeks for 5 doses of chemotherapy. Drugs commonly used include cisplaitn, carboplatin and doxorubicin. Amputation without chemotherapy can remove the source of pain, but generally metastases will become apparent in 3-4 months. Palliative therapies are those aimed at keeping the leg more comfortable so that the dog can live with it longer. There is no benefit expected in most dogs from the administration of chemotherapy drugs if the primary tumor is not removed. Radiation therapy will improve comfort in approximately 70-80% of treated dogs. Generally only a few large doses of radiation are administered. Administration of analgesics, which can be done in conjunction with palliative radiation therapy, can improve the level of comfort in some dogs. Additionally a class of drugs known as bis-phosphonates is being tried for dogs with osteosarcomas. These drugs inhibit bone resorption, or break down. They have been use in the human field for osteoporosis but also in the treatment of tumors which have metastasized to bone to relieve bone pain. Clinical trials are underway to determine if these drugs actually relieve pain in primary bone tumors of dogs. Dogs with OSA in other bone locations are often treated with a combination of surgery, radiation therapy and chemotherapy. The prognosis for dogs undergoing surgery to remove the primary limb tumor (ampuation or limb-sparing surgery) and treated with chemotherapy is fair to good. About half of dogs with OSA treated in this manner will be alive 1 year after diagnosis; approximately 25% of dogs treated in this fashion are alive 2 years after diagnosis, and occasional dogs will be cured. Dogs treated with either amputation or palliative radiation therapy live, on average, approximately 6 months before complication of the local tumor or metastatic disease cause death or prompt euthanasia. Many therapies being developed in the human field aimed at stopping metastatic disease could be helpful in dogs with osteosarcomas. Bisphosphonate drugs may also prove useful for palliation of tumor pain, particularly when combined with palliative radiation therapy. A Gene therapy trial administering a gene coding for a potent immune stimulant (IL-2) has shown promise in preliminary studies. Key points Most dogs do amazingly well with three legs; amputation, however, is not appropriate for all dogs, particularly those with other orthopedic or neurologic diseases. For such patients, palliative radiation therapy is considered an excellent treatment alternative with a high likelihood of improving patient comfort. Unfortunately, most dogs will die from complications of OSA. Statistics, while useful, can never predict how an individual dog will fare with or without specific treatment.What you might see/ Clinical presentation
Biological behavior of Osteosarcoma
Clinical staging (determination of the extent of the tumor)
Treatment options
Prognosis
Future treatment options
Other helpful sites
Seizures
A seizure is defined as a paroxysmal, transitory disturbance of brain function that has a sudden onset, ceases spontaneously, and has a tendency to recur. Generalized seizures affect the entire body. Most commonly, animals will fall to the side, make paddling movements with the limbs; they will often will urinate, salivate and defecate during the episodes. Generalized seizures usually last from several seconds to upwards of a couple minutes. Focal seizures remain localized to one body region and are usually shorter in duration, lasting a couple seconds. Seizures may start focal and then become generalized.
After the veterinarian is convinced that a seizure disorder is present, the most important question to be answered is whether the seizure is the result of primary brain disease (intracranial disease), or the result of a disturbance outside the brain (extracranial disease), The most common intracranial causes of seizures include: structural disease including hydrocephalus, head trauma, inflammatory brain disease (encephalitis), strokes and neoplasia (brain cancer). The most common causes of extracranial diseases that cause secondary brain signs include: toxins and metabolic diseases. Metabolic diseases include: low blood sugar (hypoglycemia), high blood sugar (hyperglycemia), liver disease, kidney disease, electrolyte disturbances, toxins (poisons), anemia.
Idiopathic epilepsy is another common cause of seizures in dogs and less commonly in cats. It is by definition, seizures of unknown cause. These episodes are thought to be due to "mal-wiring" within the brain. Idiopathic epilepsy is seen in dogs between the ages of 6 months and 6 years of age. It is more common in certain breeds: border collies, Australian Shepherds, Labrador retrievers, beagles, Belgian Tervurens, collies and German shepherds. That being said, seizures can occur in any breed of dog or cat. To search for the cause of seizures, a systemic work up is performed (physical and neurologic exam, blood work, blood pressure, sometimes chest x-rays, specific liver function test including bile acid testing). Once an extra-cranial cause of seizures is ruled out, then the brain is imaged using either a CT scan or an MRI. Following brain imaging, a cerebrospinal fluid (CSF) tap is performed in order to look for encephalitis. If an underlying disease can be found, then primary treatment for that disease may help to make the seizures stop. If the seizures are recurrent, anticonvulsant medications are often given. The choice of medication depends upon the characteristics of the individual animal's problem. Some of the more commonly used anticonvulsants are listed below. It is important to remember that once an anticonvulsant is initiated, it should not be changed without veterinary assistance. Most animals with idiopathic epilepsy will require anticonvulsant medication for the rest of their life. This information was made possible by funds from the Neurology Endowment at Washington State University.Idiopathic epilepsy
Drugs Used to Treat Seizures
Assistance (Service ) Dogs
Dogs can certainly be a best friend, but when they are assistance animals they are much more. These dogs allow people freedoms many of us take for granted everyday.
Rachael Armstrong is a Washington State University sophomore veterinary student at who provides "basic training" to assistance dogs. "Zack" is the two-year-old German shepherd currently under Rachael’s tutelage. His title is prominently displayed on the red vest he wears. Given his job will be to assist someone with day to day living, Zack must be exposed to every possible public environment.
It is essential for people to understand that assistance dogs, even in training, are not pets. They receive between one and two years of "basic" training exposing them to public places and then go on to "finishing" school for several more months to perfect their skills. If you encounter a person with an assistance dog there are a few simple guidelines to follow: Look at service dogs as you would any other hard working service provider, with respect for the job they are doing. This Pet Health Topic was written by Sarah Hoggan, Washington State University, Class of 2001.
Vomiting
Vomiting is a very common problem in dogs and cats. There are many causes of vomiting. Primary or gastric causes of vomiting are those that are due to diseases of the stomach and upper intestinal tract. Secondary or non-gastric causes of vomiting are caused by diseases of other organs that cause an accumulation of toxic substances in the blood. These toxic substances stimulate the vomiting center in the brain causing the animal to vomit. (Anatomy of the digestive system: dog / cat)
A problem that can be confused with vomiting is regurgitation. Vomiting is the ejection of contents of the stomach and upper intestine; regurgitation is the ejection of contents of the esophagus. The esophagus is a narrow, muscular tube that food passes through on its way to the stomach. In health, food moves quickly through the esophagus to the stomach. If the muscle of the esophagus loses tone, the esophagus dilates, a condition called megaesophagus. A dilated esophagus does not effectively move food to the stomach and the animal will regurgitate food usually shortly after eating. The food may also be inhaled into the airways causing pneumonia and cough. When you present your pet to the veterinarian because he or she is vomiting, the veterinarian will ask questions in attempt to differentiate between vomiting and regurgitation and to try to determine if your pet is vomiting due to gastric or non gastric disease. Vomiting is an active process. The pet is apprehensive and heaves and retches to vomit. If food is present in vomit, it is partially digested and a yellow fluid, bile may be present. Regurgitation is fairly passive. The animal lowers its head and food is expelled without effort. The food brought up by regurgitation is usually undigested, may have a tubular shape, and is often covered with a slimy mucus. The pet will often try to eat the regurgitated material. You may bring a fresh sample of "vomit" for the veterinarian to examine. The pH of vomit containing food is acid, the pH of regurgitated materials is higher. Your ability to answer questions about your pet's activity, habits and environment will help the veterinarian decide which causes of vomiting are most likely in your pet. A history of any drugs your pet is receiving is important. Over-the-counter pain medications such as aspirin and ibuprofen can cause severe stomach ulcers in dogs depending upon the dose and duration of treatment. The veterinarian may ask you to describe the appearance of the vomit, as well as describe how your pet looks when it vomits and the relation ship of vomiting to eating. If the vomit contains blood it may be fresh, red blood or look like coffee grounds if the blood is digested. Blood is most often seen with stomach ulcers, stomach cancer or uremia (a collection of signs including vomiting seen in pets with kidney failure). Stomach ulcers can be caused by drugs or the presence of a mast cell cancer in the skin. Mast cell cancers release histamine that leads to stomach ulcers. Regurgitation often, but not always, happens right after eating and the pet will try to eat the regurgitated food. Vomiting occurs a variable time after eating or may occur in a pet who is off food. Animals with a twisted stomach, gastric dilation-torsion, may make frequent attempts to vomit without producing anything. Pets with a hacking cough may retch and sometime vomit at the end of an episode of forceful coughing. An accurate description in this case would lead to an investigation of the causes of coughing, rather than vomiting. If your pet vomits just occasionally and has a specific series of actions associated with vomiting, you may consider video taping an episode of vomiting to help describe the episodes to the veterinarian. The physical examination of the vomiting pet can also provide information to narrow the list of possible causes. The presence of fever, abdominal pain, jaundice, anemia or abnormal masses in the abdomen will help the veterinarian make a more specific diagnosis. The mouth should be carefully examined as some foreign objects such as string can wind around the base of the tongue with the rest of the object extending into the stomach or small intestine. A nodule may be palpated in the neck of cats with hyperthyroidism. The list of non-gastric causes of vomiting is long. Pancreatitis in the dog causes vomiting that is sudden in onset and often severe. The dog may have a painful belly. Pets with pancreatitis often have a history of eating garbage or fatty table scraps. Tumors of the pancreas can cause similar signs to pancreatitis. Pancreatitis occurs in the cat but the signs are subtle and non specific and often don't include vomiting Kidney failure is a common cause of vomiting in dogs and cats. The kidneys can be acutely (suddenly) damaged by poisons such as antifreeze or by severe dehydration. Waste products that the kidneys normally get rid of, rise to high levels in just a few days. The kidneys can also gradually lose their ability to remove waste products from the body as the pet ages. Early signs of kidney failure include drinking and urinating large amounts called polyuria and polydipsia or PU-PD. PU-PD may be present for months to years before the kidney failure is severe enough to lead to waste product accumulation and vomiting. Vomiting in chronic kidney failure may began as occasional episodes and progress to severe, frequent vomiting. The pet with chronic kidney failure will often lose body condition and may have pale gums due to anemia. Non-spayed, middle aged female pets can develop a uterine infection called pyometra. Pyometra occurs within 2 months after a heat cycle and often results in discharge of pus from the vagina. The pet may frequently lick the vagina so discharge may not be seen. Dogs develop pyometra more often than cats. Other signs may include PU-PD and depression. Liver failure causes vomiting as well as other signs depending on the type of liver disease. Other signs of liver disease may include seizures, jaundice (a yellow discoloration of the areas of skin not covered by fur), PU-PD and fluid accumulation in the belly or legs. Bladder obstruction or rupture will cause a sudden onset of vomiting. The urethra that leads from the bladder to the outside can get plugged by stones or tumors. The animal will strain and pass just a few drops of urine or none at all. They will also have a painful belly. Bladder obstruction if not corrected, is fatal in just a few days. The bladder can be ruptured by blunt trauma such as being hit by a car or kicked. A form of diabetes called ketoacidosis will cause vomiting along with depression and PU-PD. Addison's disease is a deficiency of hormones from the adrenal gland and causes vomiting, diarrhea and weakness. Addison's disease occurs most commonly in young to middle aged dogs, most of which are female. Addison's is rare in the cat. The signs of Addison's disease may be intermittent or may be very severe and constant. Diseases of the inner ear can cause vomiting accompanied by incoordination, circling and tilting of the head to the side. Motion during car rides stimulates the inner ear and can cause vomiting. A sudden onset of vomiting in young, poorly vaccinated pets may be caused by infectious agents including canine distemper, canine parvovirus and feline panleukopenia virus. There are many toxins including lead, insecticides, antifreeze and other chemicals that can cause vomiting. Cats with elevated thyroid function, hyperthyroidism, may vomit in addition to other signs including, increased appetite, weight loss, hyperactivity and a poorly kept coat. Heartworm disease in cats may cause vomiting in addition to coughing, respiratory distress, weight loss and depression. Primary causes of vomiting include acute gastritis often due to eating garbage or other types of dietary indiscretions; the ingestion of large amounts of hair during grooming; ulcers of the stomach; stomach or upper intestinal cancer; parasites; food allergies; the presence of a foreign body stuck in the stomach or upper intestine; twisting and dilation of the stomach; and intussusception which is a telescoping of one part of the intestine into another piece of intestine. The stomach is usually empty 6 to 8 hours after eating. Vomiting of food when the stomach should be empty suggests an obstruction of the stomach or abnormal motion of the stomach muscles that normally grind food and push the ground food out of the stomach. Tests to differentiate primary causes of vomiting include x-rays or ultrasound of the abdomen and endoscopy. Endoscopy is the technique of passing a flexible scope into the stomach and upper intestine to examine the inside of these structures. It may be possible to remove a foreign body with endoscopy and small biopsies of the lining of the stomach and intestine can be taken for microscopic evaluation. Endoscopy requires general anesthesia. If the pet vomits sporadically, the results of all tests may be normal. Many healthy dogs and cats vomit occasionally without identifying a cause. Sometimes the cause of vomiting is as simple as the pet eating too fast. The treatment for vomiting depends upon the cause. Nonspecific treatment for vomiting includes fasting, and fluids to correct or prevent dehydration. In episodes of sudden onset of vomiting, food is withheld for 24 - 48 hours and water for 24 hours. Water should never be withheld from an animal with known or suspected kidney disease without replacing fluids intravenously or subcutaneously (under the skin). If vomiting stops, small amounts of a bland low-fat food are fed 3 to 6 times daily for a few days, with a gradual increase in the amount fed and a gradual transition to the pet's normal diet. Water is also reintroduced in small amounts on the second day. You may start with ice cubes and then gradually increase the amount of water over the day if vomiting does not reoccur. If the pet is bright and alert and has had no previous health problems, episodes of acute vomiting may be managed at home, although veterinary consultation prior to home treatment is advised. Consultation with a veterinarian in your region may reveal a recent outbreak of an infectious disease causing vomiting or identify a cluster of recent poisonings. With this type of knowledge you will want to have your pet evaluated rather than waiting a few days. Dogs and cats who vomit for longer than a few days or are depressed or dehydrated should be presented for veterinary evaluation.
Veterinary Acupuncture
Despite the fact many of its practices are thousands of years old, Eastern, or non-traditional, medicine is becoming more popular today than ever. Acupuncture is one specialized facet of non-traditional medicine that not only entered the mainstream; it’s become a treatment option for our pets.
“The specific origin of acupuncture is uncertain,” said Rodney Bagley, a veterinary neurosurgeon. “No one knows if it originally came from China, Korea, or India but it’s widely held that the Chinese perfected it.” Dr. Bagley recently completed a three-week certification course learning veterinary acupuncture techniques.
The specific mechanism of how acupuncture works is uncertain. Theories include stimulation of the release of natural chemicals with in the body or stimulation of neuromechanical mechanisms that diminish pain and promote healing. Local micro-trauma from the needle itself may also play a role. There are more than 150 acupuncture points on a dog’s body with 50-100 of those points being most commonly used. Overall, acupuncture is based on a principle of restoring balance with in the body. Veterinary ailments acupuncture is most commonly used for are pain management and diseases of the liver, kidney, and skin. Generally, acupuncture treatments are combined with traditional approaches to healing such as physical therapy or the use of medications. Just as with any medical treatment, acupuncture has innate risks associated with it. According to Dr. Bagley “There is always potential for site infection, but that’s rare because the needles used are small. Acupuncture’s effect on animals is usually positive or none at all. There have been some studies that showed it increased the growth of certain forms of cancer so it shouldn’t be used in those circumstances.” Veterinary acupuncture isn’t widely available yet. If you think it could benefit your pet ask your veterinarian for more information or a referral. Acupuncture isn’t a panacea, but it’s another tool to treat ailments and enhance the quality of our pet’s lives. Despite the amazing scientific advances in veterinary medicine, one of the most exciting new treatments may be thousands of years old.